Hip replacement surgery is one of the most successful operations performed in modern medicine. For people living with severe hip pain, stiffness, and loss of mobility, it can restore independence and dramatically improve quality of life.
In the UK, thousands of hip replacements are carried out every year through both the NHS and private sector. Yet many patients approach the operation with understandable anxiety — unsure what it involves, how long recovery takes, or whether life will truly improve afterward.
This guide explains the entire journey in clear, practical terms — from deciding whether you need surgery to what real recovery looks like months later.
When Hip Replacement Becomes Necessary
Hip replacement is usually recommended when the joint is so damaged that everyday activities become painful or difficult despite non-surgical treatment.
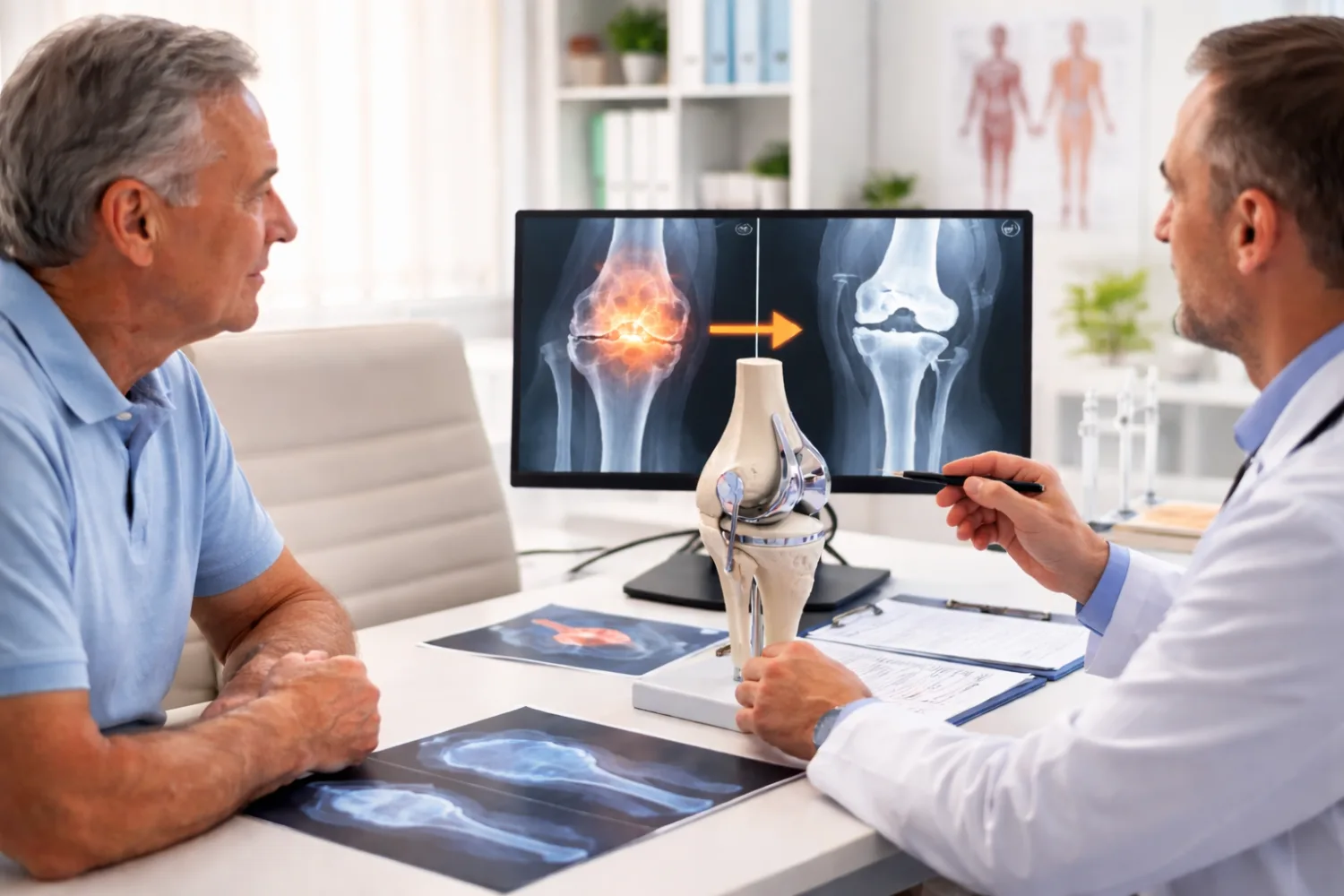
The most common cause is osteoarthritis, where the protective cartilage inside the joint gradually wears away. Bone then rubs against bone, causing pain, stiffness, and reduced movement.
People considering surgery often describe:
-
Difficulty walking even short distances
-
Pain when standing, climbing stairs, or getting out of chairs
-
Sleep disruption due to discomfort
-
Loss of independence
-
Reduced participation in work or hobbies
Many patients spend years trying physiotherapy, pain medication, lifestyle changes, or injections before surgery is suggested.
If you’re unsure whether your symptoms are severe enough, it can help to understand earlier-stage causes of joint pain. You may find our guides useful:
https://allhealthandcare.co.uk/resources/knee-pain-causes-diagnosis-treatment-in-the-uk
https://allhealthandcare.co.uk/resources/knee-replacement-surgery-in-the-uk-nhs-vs-private
Hip problems often coexist with knee or back issues, and pain can overlap.
What the Operation Actually Involves
In a hip replacement (total hip arthroplasty), the damaged joint surfaces are removed and replaced with artificial components:
-
A metal stem inserted into the thigh bone
-
A ball that replaces the top of the femur
-
A socket implanted into the pelvis
-
A smooth liner allowing friction-free movement
The goal is to recreate a smooth, stable joint that moves without pain.
Surgery usually takes one to two hours. It is typically performed under spinal anaesthetic (numbing the lower body) or general anaesthetic.
According to the NHS, the procedure replaces worn parts of the joint to improve movement and reduce pain.
Types of Hip Replacement
Most patients receive a total hip replacement, but other options may be appropriate depending on age, activity level, and overall health.
A partial replacement replaces only the ball of the joint and may be used after certain fractures, particularly in frail patients.
Some younger or very active patients may be considered for alternative procedures such as hip resurfacing, though these are less common.
Your surgeon will recommend the option most likely to give long-term benefit.
The Hospital Experience
Many people worry about the immediate aftermath of surgery. In reality, modern hip replacement pathways are designed to get patients moving quickly.
Most UK patients stay in hospital around two to three days.
Physiotherapists usually help you stand and walk within a day of surgery — sometimes within hours.
You will learn how to:
-
Walk safely using aids
-
Get in and out of bed
-
Use stairs
-
Sit and stand comfortably
-
Protect the new joint
Early mobilisation reduces complications and speeds recovery.
Recovery: What It’s Really Like
Recovery varies widely between individuals, but there is a general pattern most patients follow.
First Few Weeks
Pain and stiffness are normal at first. Swelling in the leg is common, especially if sitting for long periods.
You will likely use crutches or a walking frame and perform daily exercises to rebuild strength.
Fatigue is also common after major surgery, so pacing activities is important.
Six to Twelve Weeks
By this stage, many people are moving more confidently and gradually resuming normal activities. You may be able to return to driving and work depending on your job.
Most patients can return to usual activities within about 10–12 weeks, although recovery continues beyond that.
Three Months to One Year
Significant improvements in mobility and pain relief usually occur during this period. Many patients walk independently by three months, though progress depends on pre-operative health and commitment to rehabilitation.
Full benefit from the new joint can take up to a year.
Real-World Recovery Experiences
Patients often describe a turning point when daily pain disappears — sometimes gradually, sometimes suddenly.
A retired person who struggled to walk to local shops may regain the ability to travel, garden, or care for grandchildren.
A working adult may return to commuting and physical activity after months of limitation.
However, recovery is rarely perfectly linear. Some days feel better than others, and temporary setbacks can occur, especially after increased activity.
The most successful recoveries usually involve consistent physiotherapy, patience, and realistic expectations.
Long-Term Results
Modern hip replacements are designed to last many years. Many artificial joints function well for 15 years or more, sometimes much longer.
Most patients experience:
-
Major pain reduction
-
Improved mobility
-
Better sleep
-
Increased independence
-
Enhanced quality of life
High-impact sports and heavy manual work are usually discouraged to protect the joint, but low-impact activities such as walking, swimming, cycling, and golf are commonly encouraged.
Possible Risks and Complications
Serious complications are uncommon, but all surgery carries risks.
Potential issues include infection, blood clots, dislocation of the new joint, or wear over time. Rarely, revision surgery may be needed years later.
Some people notice a temporary sensation that one leg feels longer than the other after surgery. This usually settles as the body adapts.
Your surgical team will discuss individual risks based on age, health, and lifestyle.
NHS vs Private Hip Replacement
In the UK, both NHS and private hospitals deliver high-quality surgical care.
NHS treatment is based on clinical need and does not involve direct cost to the patient. However, waiting times can vary significantly depending on local demand.
Private treatment typically offers faster access, greater choice of surgeon, and more flexible scheduling, but involves substantial cost or insurance coverage.
Since the pandemic, many patients have opted for private surgery to avoid long waiting lists.
For a deeper comparison of treatment pathways, our guide to knee replacement surgery explores similar issues that apply to hip operations as well:
https://allhealthandcare.co.uk/resources/knee-replacement-surgery-in-the-uk-nhs-vs-private
Preparing for Surgery
Preparation plays a major role in recovery success.
Doctors commonly advise strengthening exercises before surgery, maintaining a healthy weight, stopping smoking, and optimising overall health.
Practical home preparation — such as arranging support, removing trip hazards, and organising mobility aids — can make the transition back home much smoother.
Life After Hip Replacement
For most people, the biggest benefit is not just reduced pain but regained freedom.
Patients frequently report being able to walk longer distances, travel again, participate in hobbies, and enjoy daily life without constant discomfort.
Many also notice improvements in mood and energy once chronic pain is relieved.
However, it is important to continue protecting the joint, staying active, and attending follow-up appointments to monitor long-term performance.
When to Seek Specialist Advice
If hip pain significantly limits your daily activities or continues despite treatment, a GP referral to an orthopaedic specialist may be appropriate.
Early evaluation allows time to explore non-surgical options, plan surgery if needed, and optimise health before the operation.
Final Thoughts
Hip replacement surgery can be transformative. For people whose lives have been restricted by severe joint pain, it offers a realistic path back to mobility, independence, and comfort.
While the idea of major surgery can feel daunting, modern techniques, rehabilitation programmes, and experienced surgical teams mean outcomes are generally excellent.
If hip pain is affecting your quality of life, discussing your options with a healthcare professional is the first step toward reclaiming an active future.