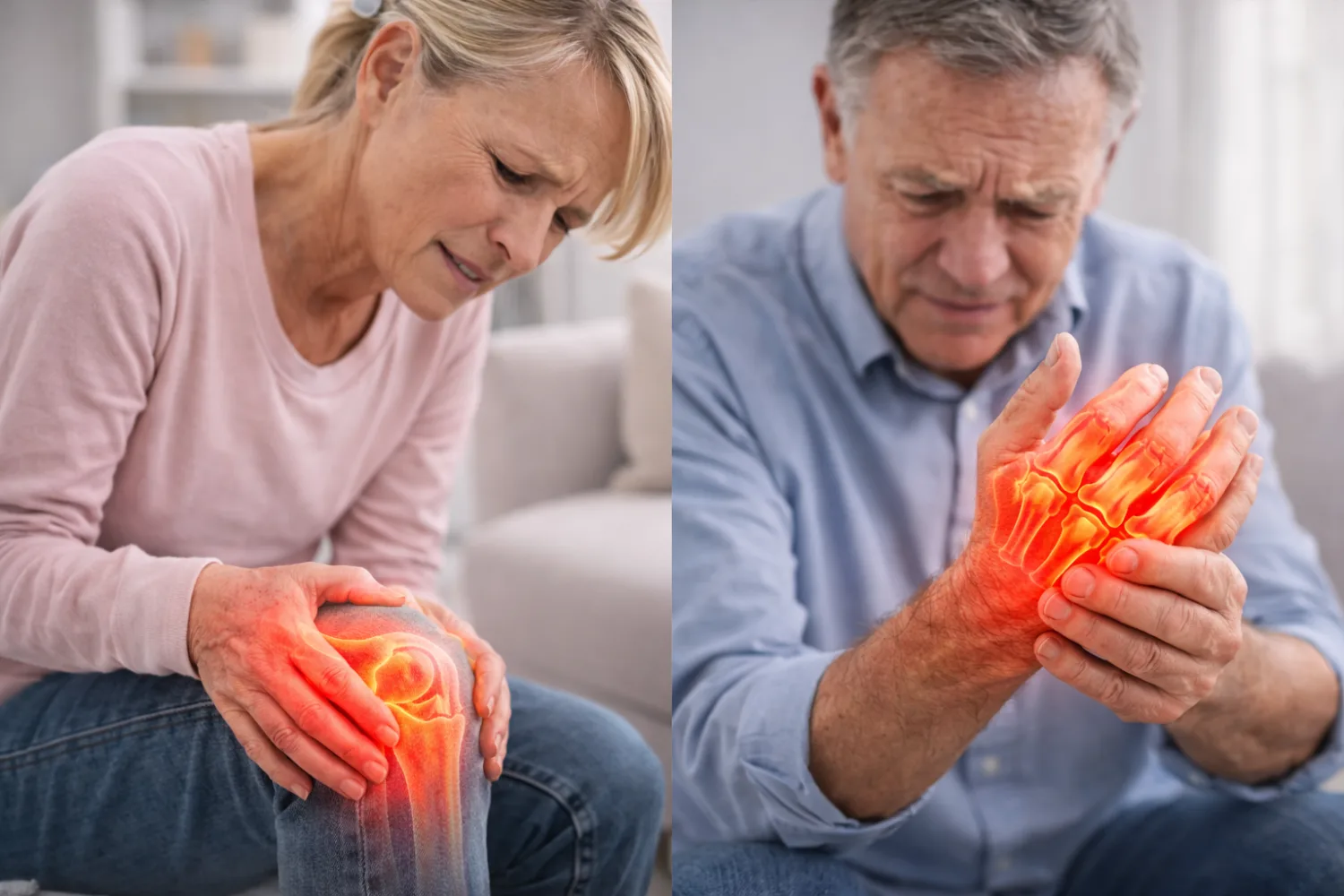
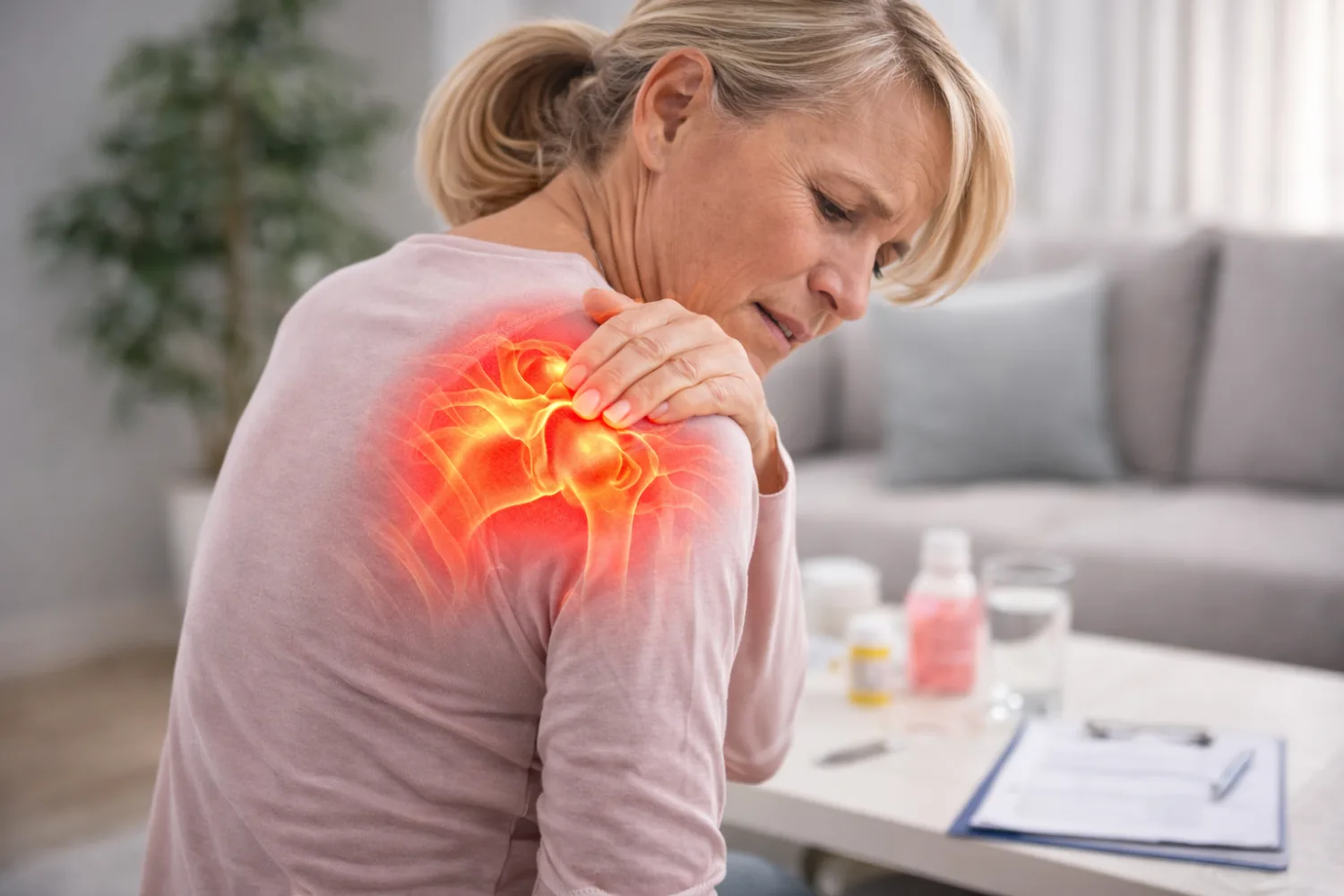
Arthritis is one of the most common long-term health conditions in the UK. It affects millions of people and is a leading cause of joint pain, stiffness, and reduced mobility. Although arthritis is often associated with ageing, it can affect adults of all ages and occasionally even younger people.
The term arthritis does not refer to a single disease. Instead, it describes a group of conditions that cause inflammation, damage, or degeneration of the joints. The two most common types are osteoarthritis and rheumatoid arthritis, which have different causes and treatments.
Understanding how arthritis develops and what treatment options are available can help people manage symptoms and maintain an active, independent life.
What Is Arthritis?
Arthritis occurs when joints become inflamed or damaged, leading to pain, stiffness, and swelling. Joints are where two bones meet, and they rely on cartilage, fluid, ligaments, and muscles to move smoothly.
When these structures become damaged or inflamed, movement becomes painful and difficult.
Arthritis commonly affects the:
-
knees
-
hips
-
hands
-
spine
-
shoulders
Over time, untreated arthritis can affect mobility and quality of life, but many treatments are available to help control symptoms and protect the joints.
The NHS provides a helpful overview of arthritis and related conditions:
https://www.nhs.uk/conditions/arthritis/
The Two Most Common Types of Arthritis
Although there are over 100 types of arthritis, two forms account for the majority of cases.
Osteoarthritis
Osteoarthritis is the most common type of arthritis in the UK.
It occurs when the protective cartilage that covers the ends of bones gradually wears down. Cartilage normally allows joints to move smoothly and absorb shock during movement. When it deteriorates, bones begin to rub against each other, leading to pain and stiffness.
Osteoarthritis most often affects weight-bearing joints such as the knees and hips, although it can also affect the hands and spine.
Common symptoms
People with osteoarthritis often experience:
Joint pain during or after activity
Stiffness, particularly in the morning
Reduced flexibility or movement
Grinding or clicking sensations in the joint
Mild swelling around the joint
Symptoms typically develop gradually over many years.
You can read more about how osteoarthritis affects the knee in our guide:
https://allhealthandcare.co.uk/resources/knee-pain-causes-diagnosis-treatment-in-the-uk
Rheumatoid Arthritis
Rheumatoid arthritis is an autoimmune disease rather than a wear-and-tear condition.
In rheumatoid arthritis, the immune system mistakenly attacks the lining of the joints, causing inflammation and swelling. Over time this inflammation can damage cartilage, bone, and surrounding tissues.
Unlike osteoarthritis, rheumatoid arthritis often affects multiple joints at the same time and commonly starts in the hands and wrists.
According to Versus Arthritis, rheumatoid arthritis occurs when the immune system attacks the joints, causing pain, swelling, and stiffness.
https://www.versusarthritis.org/about-arthritis/conditions/rheumatoid-arthritis/
Common symptoms
People with rheumatoid arthritis may experience:
Joint swelling and warmth
Morning stiffness lasting longer than 30 minutes
Fatigue and general tiredness
Symmetrical joint pain (both sides of the body)
Loss of joint function over time
Rheumatoid arthritis can also affect other parts of the body, including the lungs, eyes, and blood vessels.
What Causes Arthritis?
The causes depend on the type of arthritis.
Causes of Osteoarthritis
Osteoarthritis develops when joints gradually wear down over time. Several factors increase the risk.
Age is one of the biggest contributors. Cartilage becomes thinner and less resilient as people get older.
Joint injuries can also increase the risk of osteoarthritis later in life. Previous fractures, ligament injuries, or surgery may damage joint structures.
Other contributing factors include obesity, repetitive physical work, and genetic predisposition.
Causes of Rheumatoid Arthritis
Rheumatoid arthritis is caused by a malfunction of the immune system. Instead of protecting the body from infection, immune cells attack healthy joint tissue.
The exact cause is not fully understood, but researchers believe it involves a combination of genetic and environmental factors.
Smoking is known to increase the risk, and the condition is more common in women than men.
How Arthritis Is Diagnosed in the UK
Diagnosis usually begins with a GP consultation.
The doctor will ask about symptoms, medical history, and family history. They will also examine the affected joints for swelling, tenderness, and range of motion.
Depending on the suspected type of arthritis, several tests may be used.
Blood tests can detect inflammation markers or antibodies associated with rheumatoid arthritis.
X-rays help reveal joint damage or cartilage loss typical of osteoarthritis.
MRI or ultrasound scans may be used to detect early inflammation or structural changes in joints.
In many cases, patients are referred to a rheumatologist, a specialist in joint and autoimmune conditions.
Treatment Options for Arthritis
Although arthritis cannot always be cured, many treatments can reduce symptoms, slow progression, and improve quality of life.
Lifestyle Changes
Lifestyle changes are often the first step in managing arthritis.
Regular physical activity helps strengthen muscles around joints and maintain flexibility. Low-impact activities such as walking, swimming, and cycling are particularly beneficial.
Maintaining a healthy weight is also important because excess body weight places additional stress on joints such as the knees and hips.
Physiotherapy
Physiotherapy can help people improve movement and reduce pain.
A physiotherapist can design a personalised exercise programme to strengthen muscles and protect joints from further damage.
Exercises often focus on improving mobility, balance, and joint stability.
Medication
Medications are commonly used to control pain and inflammation.
For osteoarthritis, doctors may recommend pain relievers such as paracetamol or anti-inflammatory drugs.
For rheumatoid arthritis, disease-modifying antirheumatic drugs (DMARDs) are often prescribed to slow the progression of the disease.
In some cases, steroid injections into the joint can reduce inflammation and pain.
Surgical Treatment
When arthritis causes severe joint damage and other treatments no longer help, surgery may be considered.
Joint replacement surgery can significantly improve mobility and quality of life for people with advanced osteoarthritis.
Common procedures include:
https://allhealthandcare.co.uk/resources/knee-replacement-surgery-in-the-uk-nhs-vs-private
https://allhealthandcare.co.uk/resources/hip-replacement-surgery-in-the-uk-the-complete-guide
These surgeries replace damaged joint surfaces with artificial components that restore movement and reduce pain.
Living With Arthritis
Many people live active and fulfilling lives with arthritis.
Learning how to manage symptoms effectively is key to maintaining independence. Regular exercise, balanced activity levels, and good joint care can prevent flare-ups and maintain mobility.
Support groups and patient organisations can also provide valuable advice and emotional support.
When to Seek Medical Advice
Joint pain that lasts more than a few weeks should be assessed by a healthcare professional.
Early diagnosis is particularly important for rheumatoid arthritis because prompt treatment can prevent long-term joint damage.
If joints become swollen, warm, or difficult to move, medical advice should be sought.
Final Thoughts
Arthritis is a common condition, but it does not have to mean giving up an active life. With the right combination of treatment, lifestyle changes, and medical support, many people successfully manage symptoms and maintain good mobility.
Understanding the type of arthritis involved is the first step toward finding the most effective treatment plan.
If joint pain is affecting your daily activities, speaking with a GP or specialist can help identify the cause and guide you toward the right care.