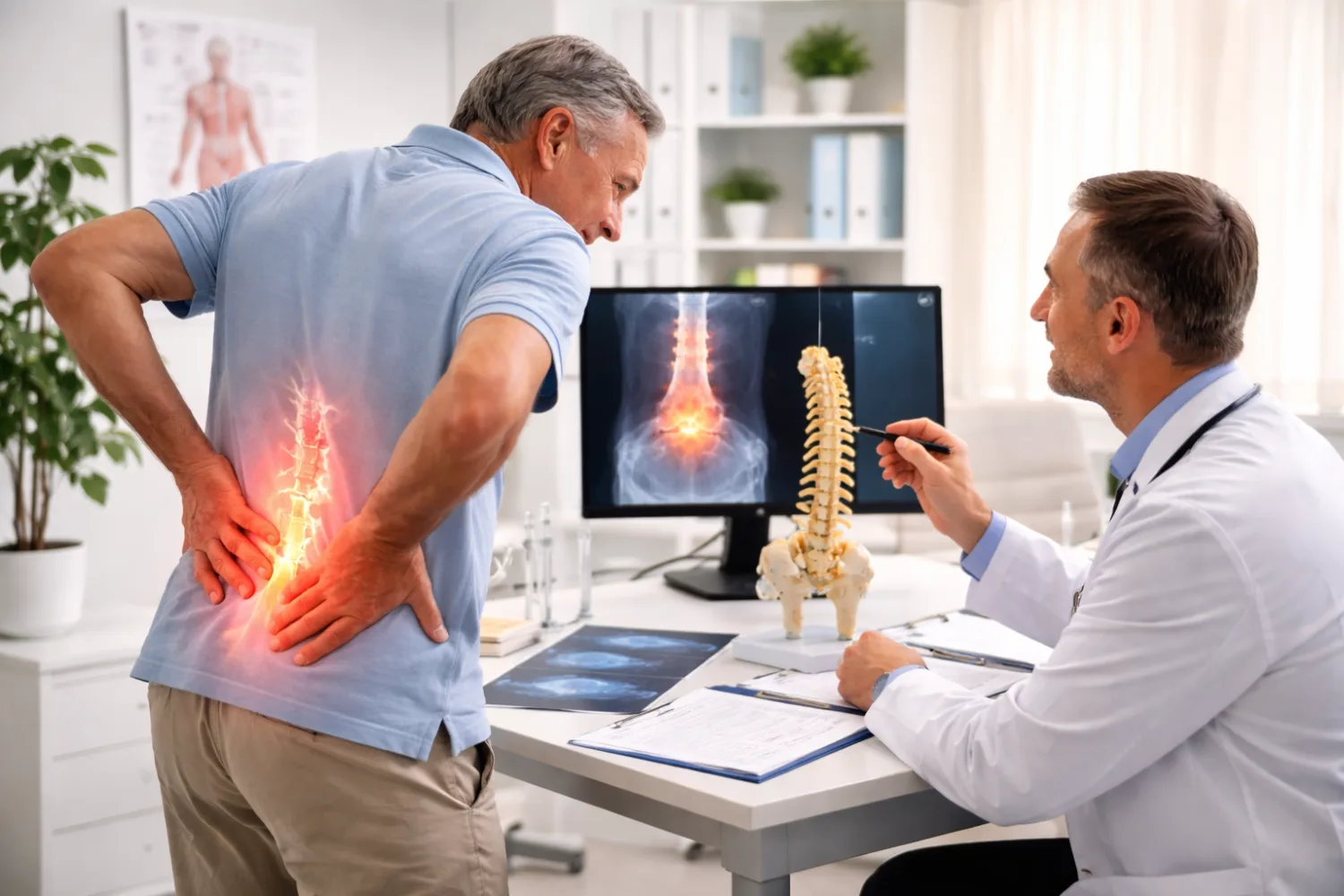
Lower back pain is one of the most common health problems in the UK. At some point in life, most adults will experience it — often more than once. For some people it appears suddenly after lifting something heavy. For others it develops gradually and becomes a persistent problem that interferes with work, sleep, and everyday activities.
The reassuring news is that most cases of lower back pain are not caused by serious disease and often improve with the right combination of movement, treatment, and lifestyle changes. Understanding why the pain occurs and how to manage it effectively is the key to long-term recovery.
This guide explains what causes lower back pain, how it is diagnosed in the UK, and what treatments are most effective based on current medical advice.
What Is Lower Back Pain?
Lower back pain refers to discomfort in the lumbar region — the lower part of the spine between the ribs and the pelvis. This area carries much of the body’s weight and plays a major role in movement, posture, and stability.
Because the spine contains bones, joints, discs, nerves, ligaments, and muscles, pain can arise from several structures at once. In many cases, doctors cannot identify a single exact cause. Instead, it is often described as non-specific lower back pain, which is the most common type.
Back pain is extremely widespread. Around 8 in 10 people experience lower back pain at some point in their lives, and it is one of the leading causes of disability worldwide.
The Most Common Causes of Lower Back Pain
Lower back pain rarely has a single explanation. Instead, several factors often combine to create symptoms.
Muscle or Ligament Strain
The most common cause of sudden back pain is a strain or minor injury to muscles and ligaments. This often happens after lifting heavy objects, awkward twisting movements, or sudden physical activity.
The pain may appear quickly or develop over several hours, often causing stiffness or muscle spasms.
Poor Movement Patterns and Inactivity
Spending long periods sitting — especially with poor ergonomics — places stress on the lumbar spine. Over time this can weaken core muscles and increase strain on spinal structures.
Research suggests that poor physical fitness, reduced muscle strength, and low activity levels are linked to back pain and its persistence.
Herniated (Slipped) Disc
Between each spinal bone sits a cushion called an intervertebral disc. When part of this disc bulges or ruptures, it may press on nearby nerves.
This condition is often called a slipped disc, although the disc does not actually “slip”. The protruding material irritates nerve roots and can cause pain that travels down the leg (sciatica).
Arthritis of the Spine
As people age, the joints and discs of the spine naturally wear down. Osteoarthritis can cause stiffness, inflammation, and chronic pain in the lower back.
This form of back pain often develops gradually and may worsen after long periods of activity or standing.
Sciatica
Sciatica occurs when the sciatic nerve — the longest nerve in the body — becomes irritated or compressed. It causes pain that radiates from the lower back down the buttock and into the leg.
Although often painful, many cases improve without surgery.
Stress and Lifestyle Factors
Pain is not purely physical. Emotional wellbeing, sleep quality, stress levels, and overall health can influence how pain develops and how long it lasts.
Factors such as anxiety, poor sleep, obesity, and smoking have all been associated with persistent back pain.
Symptoms of Lower Back Pain
Lower back pain varies widely from person to person.
Some people experience a dull, aching discomfort, while others feel sharp pain or muscle spasms. Movement may become difficult, and bending or twisting can worsen symptoms.
Pain may also spread into the buttocks or thighs, especially if nerves are irritated. In most cases the symptoms gradually improve within a few weeks.
However, sudden severe pain following injury, loss of bladder control, or numbness in the groin area requires urgent medical attention, as it could indicate a rare condition such as cauda equina syndrome.
How Lower Back Pain Is Diagnosed in the UK
Most people start by seeing their GP.
Diagnosis usually begins with questions about symptoms, lifestyle, and medical history. A physical examination may check posture, movement, and nerve function.
In many cases, scans such as X-rays or MRI are not needed. Imaging tests are usually reserved for situations where doctors suspect fractures, nerve compression, or other specific conditions.
Physiotherapists also play a major role in assessment and rehabilitation. In many areas of the UK, patients can access physiotherapy directly without a GP referral.
The Most Effective Treatments
Treatment depends on the cause of pain, but several approaches consistently help people recover.
Keep Moving
The most important advice from medical experts is simple: stay active.
In the past, bed rest was often recommended. Today, doctors know that remaining active helps the spine recover more quickly.
Gentle walking, stretching, and everyday movement encourage blood flow to injured tissues and prevent stiffness.
Physiotherapy
Physiotherapy is one of the most effective treatments for persistent back pain.
A physiotherapist can assess movement patterns and create a personalised exercise programme to strengthen the core muscles that support the spine.
These exercises often focus on improving flexibility, balance, and posture.
Pain Relief Medication
Painkillers can help people remain active while recovering.
Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, are commonly used to reduce inflammation and pain. In some cases doctors may recommend other medications if symptoms persist.
Medication is usually intended as short-term support rather than a long-term solution.
Heat and Cold Therapy
Simple treatments such as heat packs or ice packs can reduce inflammation, muscle tension, and stiffness.
Cold therapy is usually most helpful during the first few days after injury, while heat may relieve muscle tightness later.
Manual Therapy and Complementary Treatments
Some people benefit from spinal manipulation or massage provided by trained professionals such as physiotherapists, osteopaths, or chiropractors.
These therapies may provide short-term relief, particularly when combined with exercise programmes.
Lifestyle Changes
Long-term back health often depends on broader lifestyle habits.
Maintaining a healthy weight, improving sleep quality, strengthening core muscles, and managing stress can all reduce the likelihood of recurring pain.
Regular walking, swimming, and strength training are particularly beneficial.
When Surgery Is Considered
Most people with lower back pain do not need surgery. In fact, the majority of cases improve with conservative treatment.
However, surgery may be considered if:
-
nerve compression causes severe symptoms
-
mobility becomes significantly limited
-
pain persists despite months of treatment
Spinal surgery is usually reserved for specific conditions such as severe disc herniation or spinal stenosis.
Joint problems elsewhere in the body can also affect posture and spine health. For example, chronic knee or hip problems sometimes contribute to back strain. If joint degeneration is severe, procedures such as those described in our guides to
https://allhealthandcare.co.uk/resources/knee-replacement-surgery-in-the-uk-nhs-vs-private
https://allhealthandcare.co.uk/resources/hip-replacement-surgery-in-the-uk-the-complete-guide
may ultimately improve overall mobility and reduce secondary back pain.
You can also explore our detailed guide to knee pain causes and treatment here:
https://allhealthandcare.co.uk/resources/knee-pain-causes-diagnosis-treatment-in-the-uk
Preventing Lower Back Pain
Although not all back pain can be prevented, certain habits greatly reduce the risk.
Regular physical activity keeps the muscles around the spine strong and flexible. Core strengthening exercises — targeting the abdominal and back muscles — provide important support for the spine.
Good lifting technique is also essential. Always bend your knees rather than your back when lifting heavy objects.
Workstation ergonomics matter as well. Sitting with proper support, taking regular movement breaks, and adjusting desk height can help prevent strain.
Living Well With Lower Back Pain
For many people, lower back pain comes and goes over time. Even after recovery, occasional flare-ups can occur.
Learning how to manage symptoms — through movement, exercise, and stress management — is often the most effective long-term strategy.
Pain flare-ups do not necessarily mean damage is occurring. Factors such as fatigue, stress, and reduced activity can temporarily increase symptoms.
Understanding this helps many people remain confident and active rather than avoiding movement.
Final Thoughts
Lower back pain can be frustrating and sometimes frightening, particularly when it affects daily life. But the vast majority of cases are not serious and improve with the right approach.
Staying active, strengthening supporting muscles, and addressing lifestyle factors are the most effective long-term solutions.
If pain persists or worsens, seeking professional advice from a GP or physiotherapist is important. With appropriate care and guidance, most people can return to normal activities and maintain a healthy, pain-free back.