Few things make people feel more anxious than seeing a medical test result before anyone has explained it properly. A number is highlighted in red. A report says “abnormal”. A scan mentions a cyst, a lesion or “clinical correlation advised”. An ECG sounds “not quite normal”. A urine test shows blood or protein. And suddenly a result that was meant to help answer questions creates ten new ones.
This guide is here to make that experience easier.
It is a practical UK patient guide to understanding common test results, including blood tests, urine tests, ECGs, spirometry and scan reports. It explains what “normal”, “abnormal”, “borderline” and “repeat in a few weeks” usually mean, why doctors look at patterns rather than isolated numbers, and how to tell the difference between a result that needs routine follow-up and one that deserves faster attention.
The starting point is simple: a test result is rarely a verdict on its own. It is one piece of information. The NHS explains that blood tests are used to assess health, help diagnose conditions, check if treatment is working and monitor long-term problems, which is a good reminder that tests are tools, not final answers in themselves. NHS blood tests. The same logic applies across many other tests too.
Why test results are often confusing in the first place
Most medical reports are not written for patients. They are written by laboratories, radiologists or clinicians for other healthcare professionals. A scan report, for example, is often a specialist description of what can be seen on the images, followed by an interpretation for the referring doctor. RadiologyInfo notes that radiology reports are prepared for the clinician and often contain language that patients find hard to understand. RadiologyInfo: understanding your radiology report
That is why reports can sound strangely impersonal or overly technical. They are often accurate, but not always easy to live with if you read them without context.
What “normal range” really means
One of the commonest misunderstandings is the idea that any result outside the range must be bad, and any result inside the range must mean everything is fine. Real medicine is not that neat.
Reference ranges are statistical guides. Manchester NHS laboratory guidance explains that reference ranges are provided to help with interpretation and are conventionally set to cover values found in about 95% of a statistically normal population. Manchester NHS Foundation Trust reference ranges
That means two important things. First, some healthy people will naturally fall slightly outside the quoted range. Second, some people with real symptoms or disease will still have results inside the range. So “normal” does not always mean “nothing going on”, and “abnormal” does not always mean “dangerous”.
What doctors usually look at instead of just one number
When clinicians interpret results, they usually ask a series of questions:
How far outside the range is the result? Is it only just outside, or clearly abnormal? Is it part of a wider pattern with other abnormal results? Does it fit the reason the test was ordered? Has it changed from previous results? Was the patient unwell, dehydrated or on medication when the sample was taken? Does the result match the symptoms, or not?
This pattern-based way of thinking explains why a doctor may look calm about a slightly abnormal number that feels frightening to the patient, or why they may take a “normal” result seriously if symptoms remain strong.
Why repeat testing is so common
Patients often feel fobbed off when they are told to repeat a test in a few weeks or months. But repeat testing is often one of the most useful things a clinician can do.
A single result may be affected by temporary illness, dehydration, inflammation, medication, poor sampling or normal biological variation. Trend matters. NICE kidney guidance, for example, says that if eGFR is below 60 or ACR is 3 mg/mmol or higher, repeat testing after 3 months helps determine whether chronic kidney disease is really present. NICE CKD repeat testing visual summary
In other words, “repeat the test” often means “we are checking whether this is a one-off blip or a real pattern”, not “we are ignoring it”.
What “borderline” usually means
“Borderline” is not a formal diagnosis. It usually means a result sits near a threshold or only mildly outside the expected range, without giving a complete answer on its own. This is common in areas such as thyroid testing, iron studies, liver blood tests, kidney function and blood sugar.
For example, Diabetes UK says prediabetes means HbA1c is between 42 and 47 mmol/mol, which is above ideal but below the usual diabetes threshold. Diabetes UK: prediabetes. A result like that matters, but it is not the same as a clear diabetes diagnosis.
Borderline results often matter most when they fit symptoms, risk factors or a repeated pattern over time.
Blood tests: often the first place people get confused
Blood tests are probably the most common source of test-result anxiety. The NHS says blood tests are used for many reasons, including diagnosis, monitoring and assessing general health. NHS blood tests
Some of the biggest patient questions are:
What does high or low mean? Why is one result flagged but the doctor is not worried? Which result actually matters? Does a mildly abnormal result need treatment, a repeat test, or nothing at all?
If you want the full long-form guide, start here:
How to Understand Blood Test Results
That article acts as the foundation for the more specific blood test explainers below.
Liver blood tests: useful, but often misunderstood
Many people hear “your liver function tests were abnormal” and immediately assume serious liver disease. But liver panels are usually about patterns rather than one scary number. Enzymes such as ALT and AST can suggest liver-cell irritation, while tests such as ALP, GGT and bilirubin help point towards different causes or patterns. NHS Specialist Pharmacy Service explains that interpreting liver blood tests is about recognising the pattern, not just reacting to a single abnormal value. NHS SPS: interpreting liver blood tests
For a dedicated guide, read Liver Function Test Results Explained.
Kidney blood tests: the classic example of results needing context
Kidney results are a perfect example of why one number should not be over-interpreted. People often panic over creatinine or eGFR, but the NHS and NICE both emphasise that kidney assessment is based on a combination of eGFR and urine ACR, usually with repeat testing when needed. NHS chronic kidney disease diagnosis. NICE CKD assessment and management
A mildly reduced eGFR does not automatically mean kidney failure. It may need repeat testing, urine checks and a look at blood pressure, diabetes and medication history.
For the full breakdown, read Kidney Blood Test Results Explained.
Iron, ferritin and anaemia: related, but not identical
Many patients are told their iron is low when what they really mean is ferritin is low, or haemoglobin is low, or both. NICE CKS says a ferritin below 30 micrograms/L confirms iron deficiency, but ferritin can be harder to interpret when inflammation is present. NICE CKS iron deficiency anaemia
This is why someone can have low iron stores without full anaemia yet, or anaemia that is not caused by iron deficiency at all.
For the detailed guide, read Iron, Ferritin and Anaemia Blood Test Results Explained.
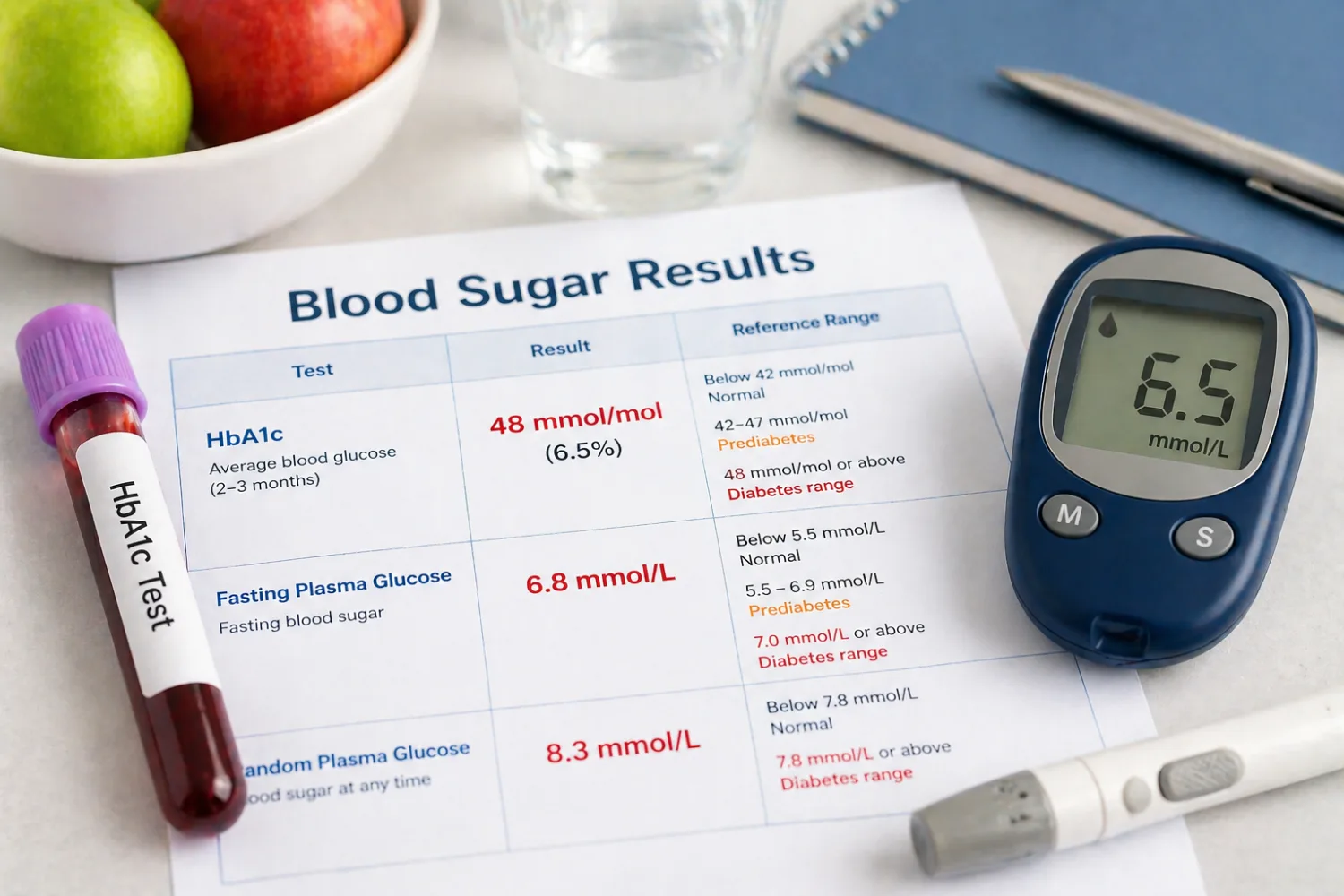
HbA1c and blood sugar: why one “high” result may not tell the whole story
Blood sugar results are another area where numbers carry a lot of emotional weight. HbA1c reflects average blood glucose over the previous two to three months, while fasting glucose is a same-day snapshot. Diabetes UK says prediabetes is 42 to 47 mmol/mol on HbA1c, and 48 mmol/mol or above is in the diabetes range. Diabetes UK: prediabetes. Diabetes UK: HbA1c
That makes blood sugar results important, but still not always final on one test alone, especially if the picture is borderline or the person has no symptoms.
For the full explainer, read HbA1c and Blood Sugar Results Explained.
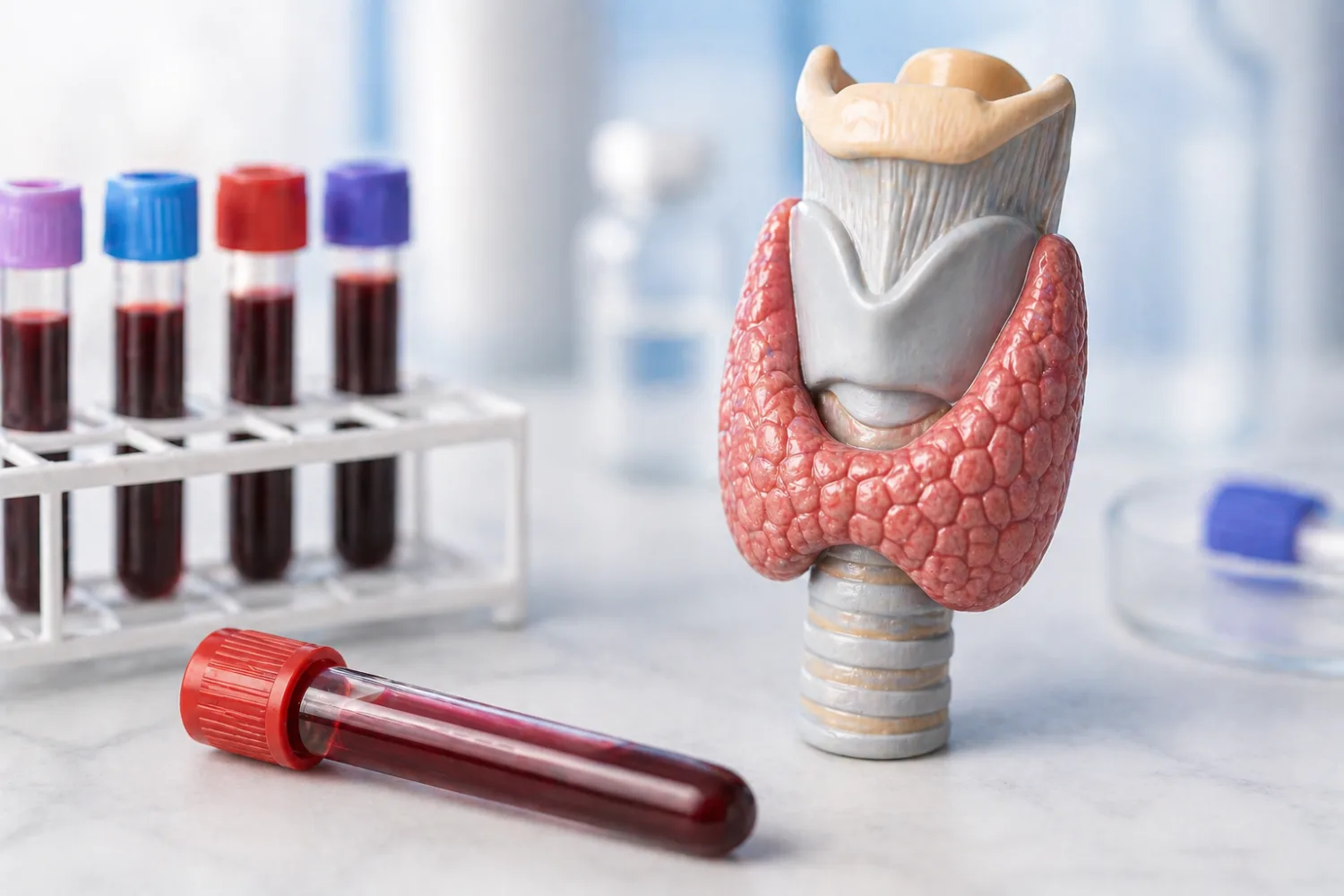
Thyroid blood tests: the classic “opposites” problem
Thyroid results confuse people because the logic feels backwards at first. In many routine cases, high TSH points towards an underactive thyroid, while low TSH points towards an overactive thyroid. The NHS and British Thyroid Foundation both explain that thyroid function tests use hormones such as TSH, T4 and sometimes T3 to diagnose underactive or overactive thyroid conditions. NHS overactive thyroid diagnosis. British Thyroid Foundation thyroid function tests
But even here, mildly abnormal results may need repeat testing and interpretation alongside symptoms and medication.
For the full explanation, read Thyroid Blood Test Results Explained.
Urine tests: simple-looking, but full of traps
Urine tests look straightforward, but they often create confusion because people assume a dipstick result is a diagnosis. It is not. Urinalysis is a screening tool that can look for blood, protein, glucose, ketones, nitrites and leukocytes, but dipsticks are not fully diagnostic on their own. NHS laboratory guidance specifically notes that urine dipstick analysis is a screening test and should be interpreted in context. Royal United Hospitals Bath urine analysis guidance
That is why nitrites and leukocytes may support a UTI, but symptoms still matter, and why blood or protein in urine often leads to follow-up rather than instant conclusions.
For the dedicated guide, read Urine Test Results Explained.
ECG results: why “abnormal” does not always mean heart disease
An ECG is one of the commonest tests used for palpitations, chest pain, dizziness and rhythm concerns. The NHS says an ECG records the electrical activity of the heart and is used to check heart rate and rhythm. NHS ECG test
But an ECG is a snapshot. It may miss intermittent symptoms if they were not happening during the test, and an “abnormal” ECG does not always mean serious heart disease. It often means the result needs to be interpreted with symptoms and sometimes other tests.
For the detailed guide, read ECG Results Explained.
Spirometry results: useful, but not the whole respiratory story
Spirometry helps show how well the lungs are working by measuring how much air you can blow out and how quickly. The NHS says spirometry is used to assess lung function and help diagnose conditions such as asthma and COPD. NHS spirometry
Key terms such as FEV1, FVC and FEV1/FVC ratio can help identify obstructive or restrictive patterns, but even here, a normal result does not always rule out asthma if symptoms are intermittent.
For the full guide, read Spirometry Results Explained.
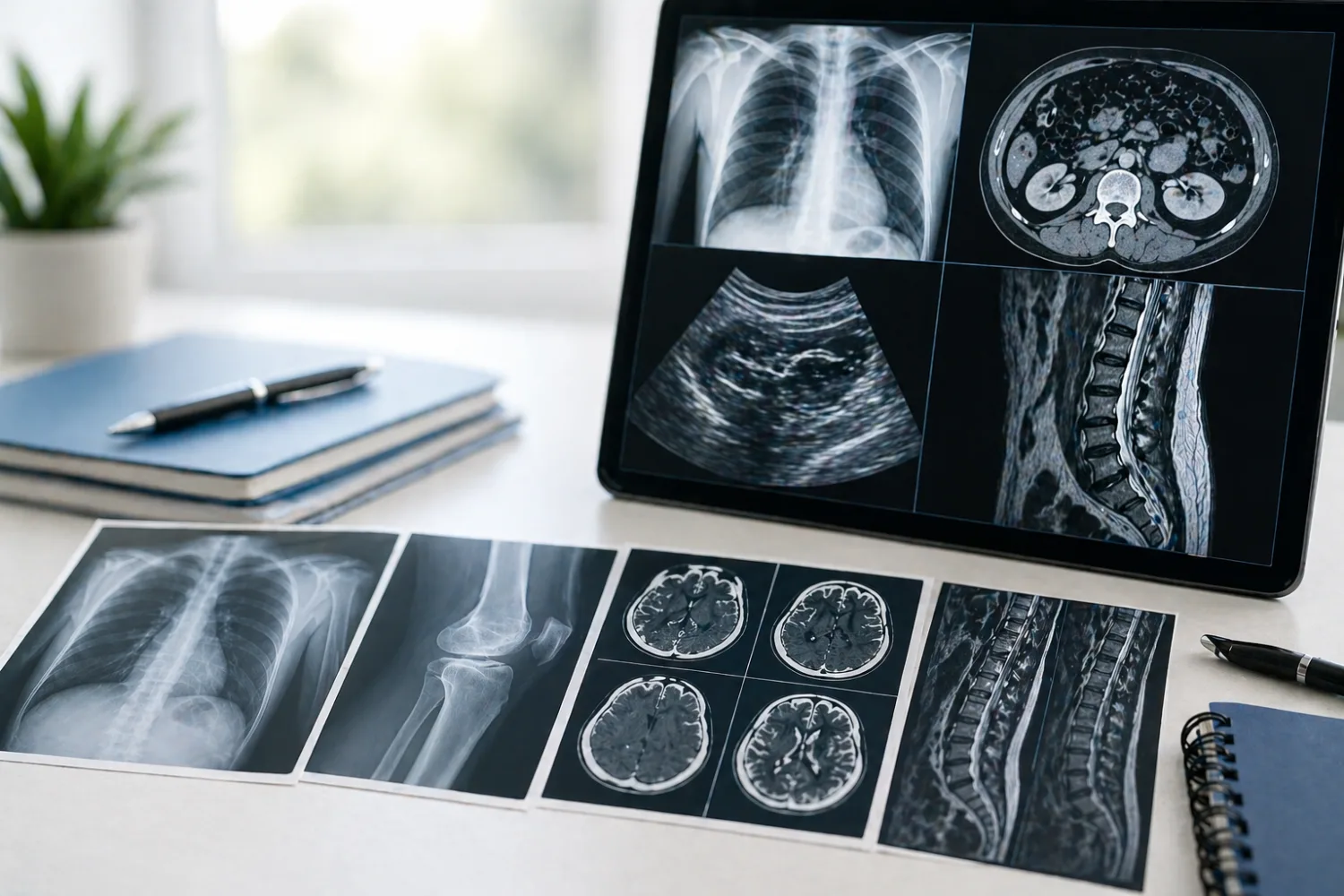
Scan reports: probably the most intimidating reports of all
Scan reports often use phrases that sound scary because they are written between clinicians. Terms such as incidental finding, no acute abnormality, clinical correlation advised, simple cyst and non-specific are common and often less alarming than they sound. RadiologyInfo explains that reports usually contain findings and an impression, and that patients often need help understanding which part matters most. RadiologyInfo: understanding your radiology report
For the detailed hub on imaging language, read How to Understand Scan Results.
What reassuring wording often looks like
No single word should be taken alone, but certain phrases often lean in a more reassuring direction. Examples include:
mild, trace, small, simple cyst, incidental, stable, no acute abnormality, no suspicious features, borderline and repeat test advised.
These do not always mean “nothing matters”, but they often suggest a finding that is limited, common, low-risk, or something that needs monitoring rather than emergency action.
What more concerning wording often looks like
Again, context is everything, but some phrases usually deserve closer attention and clearer explanation. Examples include:
marked, significantly raised, progressive, suspicious, irregular, spiculated, urgent referral, severe, declining rapidly, significant proteinuria or wording that recommends prompt specialist follow-up.
Even then, the right response is usually not internet panic, but timely follow-up with the clinician who ordered the test.
When “normal” results do not end the story
This is one of the most important things patients can understand. A normal result can be genuinely reassuring, but it does not always mean symptoms have been fully explained away. A normal ECG may miss intermittent palpitations. A normal spirometry result may not rule out asthma on a good day. A normal blood test does not rule out every digestive, hormonal or musculoskeletal condition. The test may still have done something useful by ruling out one category of problems, even if it did not provide the final answer.
This is why the best follow-up question is often not “Was it normal?” but “What does this result rule out, and what does it not rule out?”
When abnormal results need quicker action
Most abnormal results are not emergencies. But some test-result situations should be followed up promptly, especially if they come with concerning symptoms.
Examples include chest pain with abnormal ECG or cardiac blood tests, rapidly worsening kidney results, severe anaemia, jaundice with abnormal liver tests, blood in urine or stool, signs of infection with significant abnormality, or a scan report that specifically recommends urgent review.
Symptoms still matter as much as the test. A mildly abnormal result in a well person may be much less urgent than a borderline result in someone who is very unwell.
Questions worth asking after any test result
If you only remember one practical section from this article, make it this one. These are the questions that usually help most:
What was the test looking for in the first place? Which result matters most? Is this mildly abnormal or clearly significant? Does it need repeating? Does it fit my symptoms? Could it be temporary? Do I need treatment, monitoring or another test? What symptoms should make me seek help sooner?
Those questions work for bloods, urine tests, ECGs, spirometry and scans. They are much more useful than simply asking whether the result was “good” or “bad”.
Where to go next in this test-results guide series
If you want a deeper explanation of a specific result type, these are the best next reads:
How to Understand Blood Test Results
Liver Function Test Results Explained
Kidney Blood Test Results Explained
Iron, Ferritin and Anaemia Blood Test Results Explained
HbA1c and Blood Sugar Results Explained
Thyroid Blood Test Results Explained
Urine Test Results Explained
ECG Results Explained
Spirometry Results Explained
How to Understand Scan Results
The bottom line
The best way to understand medical test results is not to treat them like exam marks. They are not pass or fail. They are pieces of information. Some are reassuring. Some are clues. Some need repeating. Some clearly point towards a diagnosis. And many only make sense when combined with symptoms, history and the reason the test was done in the first place.
If you remember the core principles, you will already be ahead of most people reading their results online:
normal does not always mean “nothing is wrong”; abnormal does not always mean “something serious is wrong”; repeat testing is often sensible; patterns matter more than isolated numbers; and the most important question is usually not “what does this word mean?” but “what does this result actually mean for me?”
Frequently asked questions
Does an abnormal test result always mean something serious?
No. Many mildly abnormal results turn out to be temporary, low-risk or only significant when combined with other findings. Reference ranges are guides rather than perfect yes-or-no cut-offs, and some healthy people will fall slightly outside them. Manchester NHS Foundation Trust reference ranges
Why do doctors repeat tests instead of treating straight away?
Because one result may not show whether a problem is temporary or persistent. Repeat testing often helps separate a short-term blip from a real pattern. NICE kidney guidance is a clear example of this approach. NICE CKD repeat testing visual summary
What does “borderline” usually mean?
It usually means the result is close to a threshold or only mildly outside the expected range. It may matter, but often needs context, trend and sometimes repeat testing rather than instant conclusions.
Can results be normal even if I still feel unwell?
Yes. Normal tests can be reassuring, but they do not rule out every condition, and some problems are intermittent or not easily captured by one test. That is why symptoms still matter.
What is the most useful question to ask after getting a test result?
Ask what the test was looking for, whether the result answers that question, whether it needs repeating, and what happens next. That usually gets a more helpful answer than just asking whether the result was “good” or “bad”.
When should I seek help sooner rather than waiting for routine follow-up?
Seek quicker medical advice if abnormal results come with concerning symptoms such as chest pain, severe breathlessness, jaundice, heavy bleeding, visible blood in urine, black stools, confusion, severe weakness or rapid worsening illness.
Why do scan reports sound so technical?
Because they are written mainly for clinicians. RadiologyInfo explains that radiology reports are specialist reports designed to help the referring doctor interpret the findings. RadiologyInfo: understanding your radiology report
Is one test ever enough for a diagnosis?
Sometimes yes, but often no. Many diagnoses are made using a combination of symptoms, examination, bloods, scans, repeat testing and follow-up over time rather than one isolated result.