Scan reports can be deeply unhelpful when you read them for the first time. They often contain phrases that sound serious, vague or both at once: “no acute abnormality”, “incidental finding”, “clinical correlation advised”, “degenerative change”, “simple cyst”, “non-specific”, “lesion”, “mild prominence”, “further imaging may be considered”. None of these phrases are written to reassure ordinary patients. They are written as communication between clinicians. RadiologyInfo explains that radiologists interpret imaging tests and write reports for the referring clinician, and that these reports often contain complex language that can be hard for patients to understand.
This guide explains how scan reports are structured, what common phrases often mean, and how to think about results from ultrasound, X-ray, CT and MRI without jumping to the worst conclusion. It is written for UK patients, but the language used in radiology reports is similar across many healthcare systems. The aim is not to replace your clinician’s explanation. It is to help you understand the report well enough to ask better questions.
What scan reports are actually for
A scan report is not the same thing as a diagnosis. It is a specialist description of what the radiologist can see on the images, plus an interpretation of how those findings may or may not fit the clinical question. RadiologyInfo notes that a typical radiology report includes the type of exam, a description of findings, and an impression or summary to help the referring clinician understand what matters most.
This is why reports can feel oddly unsatisfying when patients read them directly. A radiologist may describe several things seen on the scan, but the clinician looking after you still has to decide which of those things are important, which are incidental, and whether the findings actually explain your symptoms. A scan can show an abnormality that turns out to be harmless. It can also be technically normal but still not fully rule out every possible cause of symptoms, depending on the body part and the question being asked.
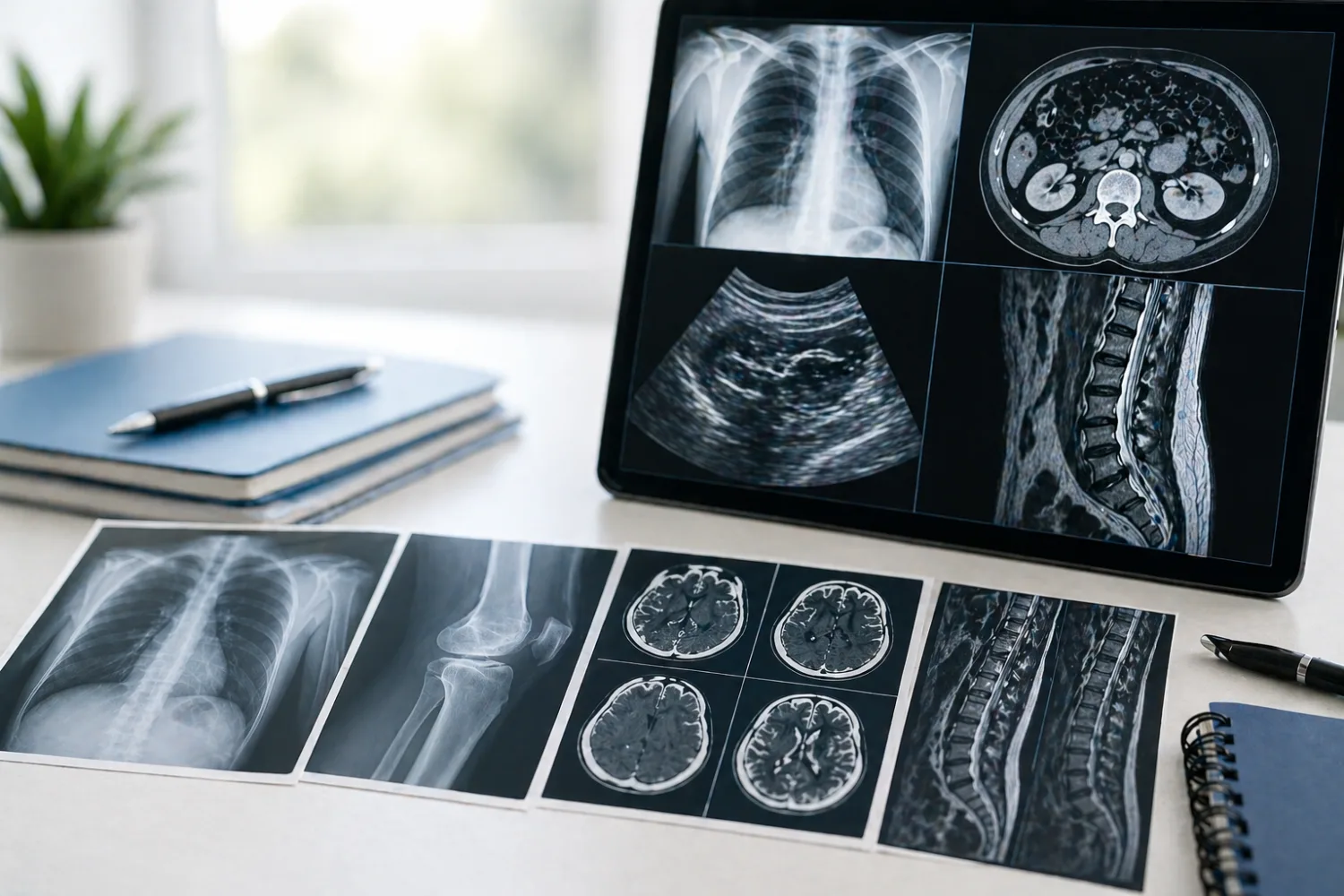
The basic difference between ultrasound, X-ray, CT and MRI
It helps to know what each scan is good at. An X-ray is usually best for bones and some chest problems. A CT scan uses X-rays to create more detailed cross-sectional pictures inside the body. The NHS says CT scans take detailed pictures of the inside of the body and are usually used to diagnose conditions or check how well treatment is working.
An ultrasound uses sound waves rather than radiation and is often used for the abdomen, pelvis, pregnancy, soft tissues and blood flow questions. NHS patient information from imaging departments explains that ultrasound is performed in radiology departments and community settings by sonographers or doctors and is commonly used to examine internal organs and structures.
An MRI uses magnetic fields and radio waves to produce highly detailed images, especially of soft tissues, joints, spine, brain and some internal organs. RadiologyInfo explains that MRI provides detailed images of internal structures and can image soft tissues from many angles.
These differences matter because the same phrase can carry different weight depending on which scan was used. A “lesion” on ultrasound may lead to CT or MRI for better characterisation. A normal X-ray may still be followed by MRI if the concern is more about soft tissue than bone.
How most scan reports are structured
Although the wording varies, many radiology reports follow a similar structure. There is usually a heading that states the type of exam, then a section describing the findings, and finally an impression or summary. RadiologyInfo’s patient guide to radiology reports describes these same broad sections and explains that the impression is often the most important summary for the referring clinician.
If you are reading your own report, it often makes sense to read the findings first, then go back and focus on the impression. The findings may contain lots of detail that is not actually the key message. The impression is usually where the radiologist says, in effect, “this is what I think matters most”.
What “no acute abnormality” means
This is one of the commonest phrases patients see, especially on emergency or urgent scans. In plain English, it usually means the scan did not show an obvious new urgent problem that needs immediate action. It does not necessarily mean the scan was completely normal in every respect.
For example, someone may have a CT done in hospital and the report says “no acute abnormality”, but the same report may also mention mild fatty liver, old degenerative spinal change, a simple cyst or some chronic sinus thickening. “No acute abnormality” usually means nothing dramatic or time-critical was seen on that scan, not that the body was found to be perfectly textbook normal.
What “incidental finding” means
An incidental finding is something seen on the scan that was not the main reason the scan was done. RadiologyInfo explains that radiologists sometimes see abnormalities outside the main area or question being assessed, and these are called incidental findings.
This is a very common source of anxiety because patients often think, “If they found something unexpected, it must be dangerous.” In reality, many incidental findings are harmless or low-risk. A simple kidney cyst, a small liver cyst, mild age-related wear-and-tear in the spine, or a small benign-looking thyroid nodule may all be incidental findings.
The important question is not “Was it incidental?” The important question is “Does the report say it looks benign, and does it need follow-up?” Many incidental findings do not need anything more than awareness. Some do need another scan, a blood test or interval monitoring. The wording usually gives clues.
What “clinical correlation advised” means
This phrase frustrates patients because it sounds like a non-answer. What it usually means is that the scan finding needs to be interpreted alongside your symptoms, examination and other test results. In other words, the image alone does not settle the whole question.
A radiologist may be able to say, “There is mild thickening,” “There is a small amount of fluid,” or “There are degenerative changes,” but whether that actually explains your pain, cough, dizziness or bloating depends on the wider clinical picture. “Clinical correlation advised” often means the radiologist is being appropriately cautious rather than evasive.
What “non-specific” means
Non-specific usually means the finding is real enough to mention, but it does not point neatly to one diagnosis. This is a very common radiology phrase. For example, “non-specific bowel wall thickening”, “non-specific white matter change” or “non-specific inflammatory change” tells the clinician that something is seen, but the imaging pattern is not distinctive enough on its own to confidently name the cause.
Patients often read “non-specific” as “they have no idea”. That is not quite right. It usually means “we can see a change, but this appearance is shared by more than one possible explanation”.
What “lesion” means
Lesion is one of the most frightening words in a scan report, but it is also one of the broadest. In radiology language, a lesion simply means an area that looks different from the surrounding tissue. It does not automatically mean cancer. It could refer to a cyst, a benign nodule, a scar, an area of inflammation, a bruise, a tumour or another structural change.
That is why the words around “lesion” matter so much. “Simple cystic lesion” sounds very different from “solid enhancing lesion” or “indeterminate lesion”. Patients should train themselves not to react to the word lesion in isolation.
What “simple cyst” usually means
This is one of the most reassuring phrases in imaging. A simple cyst usually means a fluid-filled sac with features that look straightforward and benign. RadiologyInfo’s patient guidance on renal cysts explains that simple kidney cysts are common, especially in older people, and are usually harmless.
Simple cysts can be found in the kidneys, liver, ovaries and other organs. They are often incidental findings and, depending on the organ and context, may not need treatment at all. This is a good example of why a scan can find something real without that thing being dangerous.
What “mild”, “minimal” and “small” usually suggest
Radiology reports often use scale words such as mild, minimal, small, trace or tiny. These words are not perfect, but they usually suggest the radiologist is describing something limited rather than extensive. “Mild degenerative change”, “small effusion”, “trace free fluid” or “minimal mucosal thickening” usually sound less worrying than more aggressive wording such as “marked”, “large”, “extensive” or “suspicious”.
That does not mean mild findings are always irrelevant. A small stone in the wrong place can still cause severe pain. Mild inflammation may still fit symptoms. But the tone and scale words in a report do often give a useful clue about how concerning the radiologist thinks the appearance is.
What “degenerative changes” means
This phrase shows up constantly on X-rays, CTs and MRIs of the spine and joints. In plain English, degenerative changes usually means age-related wear-and-tear changes such as disc dehydration, small bone spurs, joint narrowing or arthritic change. It often sounds more serious than it really is.
A very common example is someone with back pain whose MRI mentions “mild multilevel degenerative changes”. That may sound dramatic if you are imagining degeneration as something catastrophic. In practice, it often means fairly common age-related change, some of which may or may not be responsible for symptoms.
This type of report wording would link naturally with your existing articles on lower back pain, sciatica, herniated or slipped disc and arthritis explained.
Common ultrasound report terms
Ultrasound reports often include words such as echogenic, hypoechoic, anechoic, solid, cystic and vascularity. Patients do not need to memorise these, but a few broad ideas help.
Cystic usually suggests fluid. Solid means tissue rather than simple fluid. Anechoic often goes with simple fluid. Vascularity refers to blood flow within a structure. These descriptions help the radiologist classify what kind of thing they are seeing, which is why an ultrasound report may lead to phrases like “simple cyst”, “solid nodule” or “indeterminate lesion requiring further characterisation”. RadiologyInfo’s patient guide to abdominal ultrasound reports explains that reports describe what was seen and how it is characterised rather than instantly giving a diagnosis in every case.
Ultrasound is especially prone to follow-up wording such as “correlate clinically” or “consider further imaging” because some structures are not fully characterised by ultrasound alone.
Common X-ray report terms
X-rays are often used for bones, joints and the chest. Common report language includes fracture, dislocation, consolidation, effusion, no focal abnormality, degenerative change and no acute bony injury.
In chest X-rays, consolidation often refers to an area that may represent infection such as pneumonia. Pleural effusion means fluid around the lung. No focal consolidation is generally reassuring if pneumonia is the concern. In bone or joint X-rays, “no acute bony abnormality” usually means no new fracture or dislocation was seen.
Because X-rays are less detailed than CT or MRI, reports may also mention that findings are limited or that further imaging is needed if symptoms persist.
Common CT report terms
CT reports often include terms such as attenuation, enhancement, calcification, fat stranding, mass effect, lymphadenopathy and incidental lesion. RadiologyInfo’s patient information on reading CT reports notes that common report terms can include things like hypoattenuating lesions and other descriptors patients find confusing.
Enhancement usually refers to how tissue behaves after contrast is given. Calcification means calcium is visible in a structure. Fat stranding often means inflammatory change in surrounding fat. Lymphadenopathy means enlarged lymph nodes. None of these words automatically means cancer, but some carry more weight than others depending on the context and what else is seen.
CT is often used when clinicians need more detail than an X-ray can give, especially in the head, chest, abdomen and pelvis. The NHS says CT scans provide detailed pictures inside the body and are often used to diagnose conditions or assess treatment.
Common MRI report terms
MRI reports often use terms such as signal, high signal, low signal, disc bulge, nerve root impingement, marrow oedema, white matter change, tear, oedema and enhancement. MRI is especially detailed for soft tissues, which is why its reports can feel particularly technical. RadiologyInfo explains that MRI gives detailed pictures of soft tissues and structures from multiple angles.
A phrase like “small disc bulge” is often less dramatic than patients fear. “Nerve root compression”, on the other hand, may fit symptoms such as sciatica more closely. “White matter changes” in brain MRI reports are another example of wording that often sounds alarming but can reflect several possible explanations, including age-related or vascular changes, depending on the patient and the pattern.
What “further imaging recommended” means
This usually means the radiologist has seen something that is not fully characterised on the current scan and believes another imaging test would answer the question better. For example, a lesion seen on ultrasound may need CT or MRI to clarify whether it is a simple cyst, a haemangioma, or something else. This does not automatically mean the finding is ominous. Sometimes it simply reflects the limits of the first imaging method.
Patients often interpret “further imaging recommended” as “they are worried this is cancer”. Sometimes cancer is one possibility among several, but often the recommendation is simply because the first scan cannot describe the finding precisely enough.
What “compare with previous imaging” means
Radiologists often want to know whether a finding is new, stable or changing. A small nodule or cyst that has looked identical for years is often much less concerning than one that has clearly grown. This is why older scans can be surprisingly important. Stability over time is often reassuring, while change over time may push the clinician towards more follow-up.
How to tell whether a report sounds reassuring or more concerning
Patients often want a simple way to judge tone. While nothing replaces clinical explanation, some wording is generally more reassuring than others.
Words such as simple, benign-appearing, stable, mild, trace, incidental, no acute abnormality and no suspicious features often lean in a more reassuring direction.
Words such as indeterminate, suspicious, irregular, spiculated, enhancing mass, lymphadenopathy, progressive or urgent referral recommended tend to sound more significant and usually deserve fuller explanation and follow-up.
But it is still the pattern that matters, not one loaded word in isolation.
Why scan findings do not always explain symptoms
This is one of the most important reasons patients get disappointed or confused by reports. A scan may show something real that turns out not to be the cause of symptoms. Equally, a scan may be reported as normal or only mildly abnormal while symptoms are still very real. Imaging is powerful, but it does not answer every question. That is why clinicians often combine scan results with blood tests, examination, history and other investigations.
This article fits naturally with your other explainers, especially how to understand blood test results, ECG results explained, urine test results explained and spirometry results explained. Together they help patients understand that test results nearly always need context.
Questions worth asking after you read a scan report
If you have read a report and still feel unsure, the best questions are usually:
What was the scan mainly looking for? Did it answer that question? Which finding matters most? Is anything incidental? Does anything need follow-up? If so, what sort and when? Does this actually explain my symptoms? Is comparison with older imaging important? Are any urgent features present?
Those questions are much more useful than asking, “Is my scan bad?” because scan reports are rarely that black and white.
The bottom line
The most important thing to understand about scan reports is that they are written as specialist descriptions, not as direct patient advice. Terms such as incidental finding, no acute abnormality, non-specific change, simple cyst and clinical correlation advised often sound more worrying than they really are. RadiologyInfo’s guide to radiology reports emphasises that reports can be complex and that patients often need help understanding which parts are most important.
A good rule is this: do not react to one word in isolation. Look at the overall impression, the tone, whether follow-up is recommended, and whether the report actually answers the question the scan was ordered to investigate. That is usually where the real meaning sits.
Frequently asked questions
What does “no acute abnormality” mean on a scan report?
It usually means no obvious new urgent problem was seen on the scan. It does not necessarily mean every part of the scan was completely normal.
What is an incidental finding?
An incidental finding is something seen on the scan that was not the main reason the scan was done. Many incidental findings are harmless or low-risk, though some need follow-up. RadiologyInfo explains that incidental findings are abnormalities seen outside the original reason for the exam.
Does “lesion” mean cancer?
No. In radiology, “lesion” is a broad word for an area that looks different from the surrounding tissue. It can refer to many things, including benign cysts, inflammation, scars or tumours.
What does “clinical correlation advised” mean?
It usually means the scan finding needs to be interpreted alongside your symptoms, examination and other test results. The image alone does not fully answer the question.
What does “simple cyst” mean?
It usually means a fluid-filled sac with benign-looking features. RadiologyInfo explains that simple kidney cysts, for example, are common and usually harmless.
Why does my report mention “degenerative changes”?
This usually refers to age-related wear-and-tear changes in bones, joints or discs. It often sounds more dramatic than it is, though it may still be relevant depending on your symptoms.
What does “further imaging recommended” mean?
It usually means the radiologist has seen something that cannot be fully characterised on the current scan and another scan type may describe it better. It does not automatically mean the finding is serious.
Can a scan be normal even if I still have symptoms?
Yes. A normal scan can be reassuring, but not every symptom has a visible imaging explanation. That is why scan results are interpreted alongside the rest of the clinical picture.