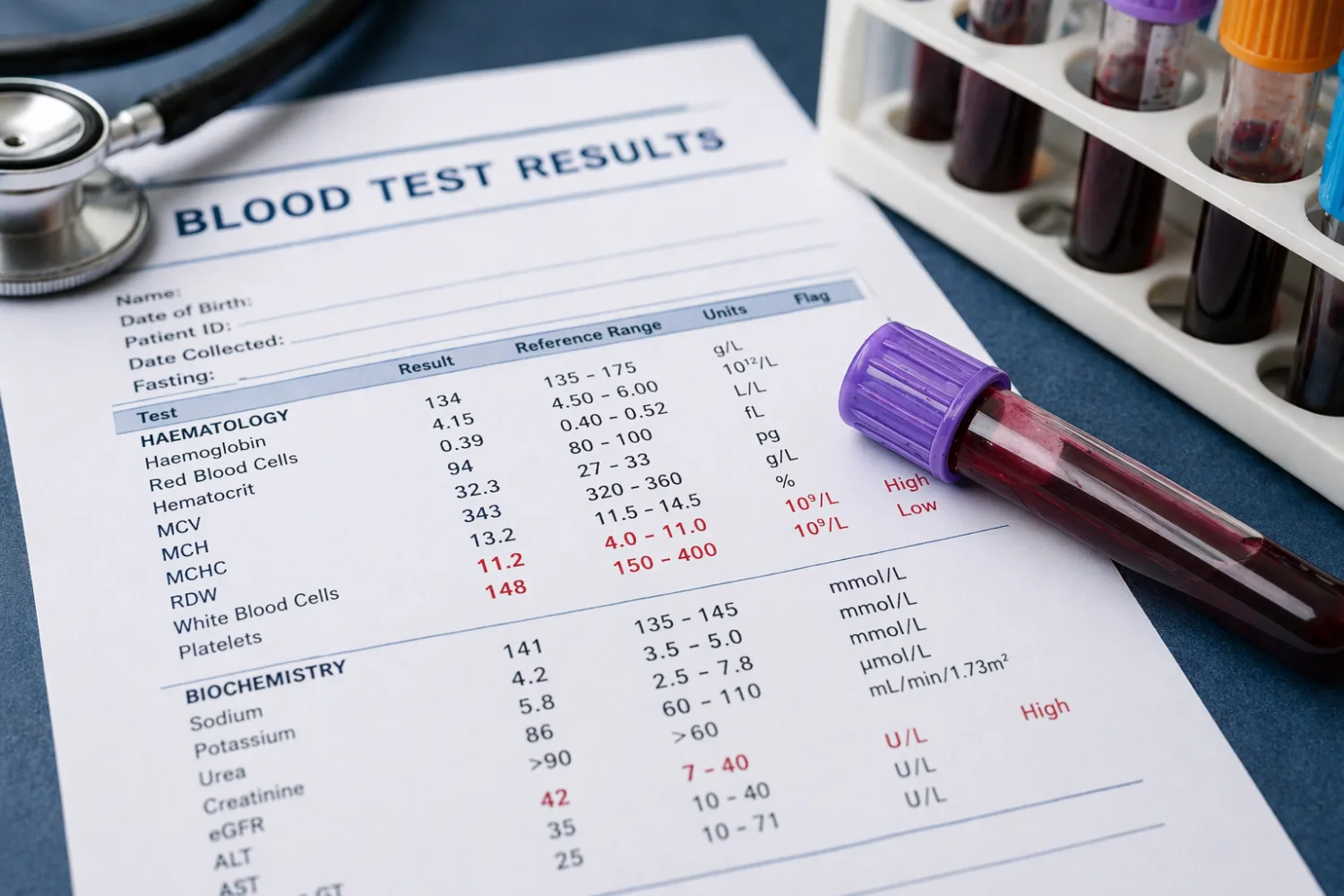
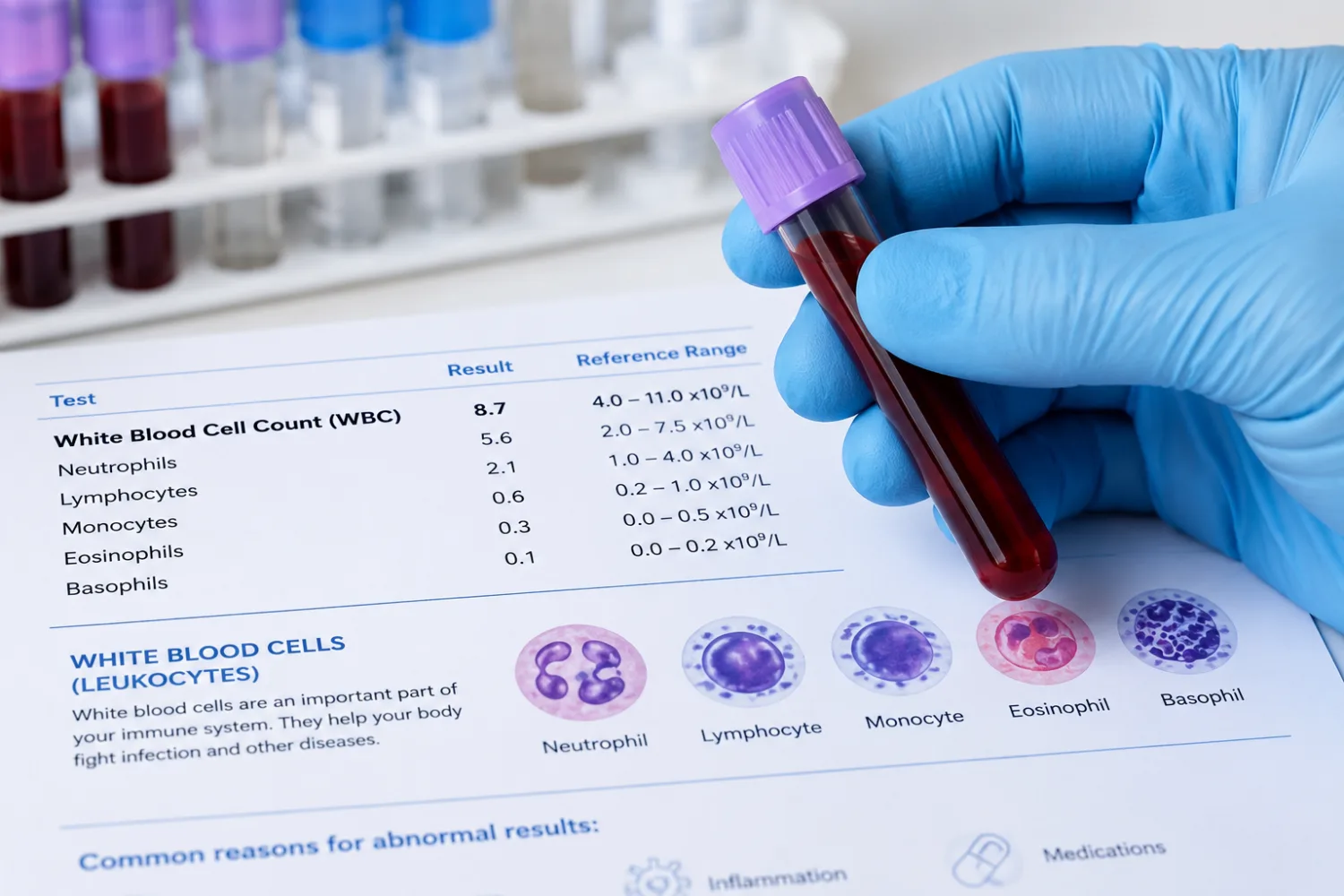
Few things create more low-level anxiety than opening a blood test report and seeing a line of abbreviations, numbers and little arrows pointing up or down. It is one of the most common modern health experiences: you had a blood test because you were tired, worried about symptoms, having a routine check, starting medication, or following up on a long-term condition. A few days later the results appear in an app, a text message arrives, or the surgery tells you that “some of the bloods were slightly abnormal”.
Then the guessing begins.
Is a result just outside the range a problem? If one number is marked red, does that mean something is wrong? Why would a GP say “nothing urgent” if the report says abnormal? And how are ordinary patients supposed to make sense of terms like FBC, HbA1c, eGFR, ALT or ferritin?
This guide is here to make that much easier. It is written for UK patients and explains the blood tests people most often see in plain English. It will help you understand what the common tests measure, what high or low results can suggest, what a “normal range” really means, and when a result deserves follow-up rather than panic.
The starting point is reassuring but important: blood tests are incredibly useful, but they are almost never the whole story. The NHS blood tests overview explains that blood tests are used to assess general health, help diagnose conditions, check if treatment is working and monitor longer-term problems. In other words, blood tests are tools. They help clinicians build a picture. They do not replace symptoms, examination, medical history or common sense.
What a blood test can and cannot tell you
Blood tests are good at spotting patterns. They can show evidence of anaemia, inflammation, diabetes risk, kidney strain, thyroid imbalance, vitamin deficiency, liver irritation and much more. They can also help monitor how a condition is changing over time, or whether a treatment is helping.
But blood tests often do not give a complete diagnosis on their own. A mildly raised liver enzyme does not automatically tell you why it is raised. A low ferritin may suggest low iron stores, but it does not by itself explain the cause. A raised white cell count may happen with infection, inflammation, stress, medication effects and other الأسباب. The meaning comes from the context.
This is why doctors do not usually interpret one isolated number in a vacuum. They look at the pattern, how abnormal it is, whether it fits your symptoms, whether it has changed from previous results, whether you were unwell when the test was taken, what medicines you take, and what conditions you already have.
A useful way to think about blood tests is this: they are often better at narrowing down possibilities than handing you a neat answer.
How to read a blood test report without panicking
Most UK blood test reports show the name of the test, your result, the laboratory’s reference range, and sometimes a flag for “high” or “low”. That looks simple enough, but it is often misleading in practice because patients naturally assume that “outside the range” equals “serious problem”. It does not work that way.
Reference ranges are based on what is typical for most healthy people in that laboratory’s population. That means a result can fall just outside the stated range and still be clinically unimportant. Equally, a result can sit technically within range and still matter if it is changing, if it does not fit your usual pattern, or if it matches a particular symptom story.
A very ordinary example is a mildly raised white cell count during or just after a cold. Another is a slightly borderline liver enzyme after recent illness, alcohol, strenuous exercise or medication use. Another is a ferritin result that is “normal” on paper but low enough, in the right context, to fit iron deficiency symptoms.
So before reacting to a single flagged value, ask better questions:
How far outside range is it? Is it a tiny difference or a large one? Is it part of a pattern with other results? Has it happened before? Does it fit why the test was done? Was I ill, dehydrated, fasting, menstruating, pregnant or taking medication at the time?
Those questions are much closer to how clinicians think.
Why “normal” does not always mean perfect, and “abnormal” does not always mean dangerous
This is one of the most important parts of understanding blood tests.
A “normal” result means the test did not show a significant abnormality according to that lab’s range and method. It does not necessarily prove that nothing at all is wrong. For example, someone with symptoms of coeliac disease, endometriosis, IBS or early inflammatory disease may still have several blood results within normal range. Blood tests are useful, but they are not magic.
An “abnormal” result, on the other hand, may be minor, temporary or simply something that needs repeating before anyone jumps to conclusions. This is especially common with mildly abnormal liver tests, borderline inflammatory markers, small white cell changes, slightly low sodium, or kidney numbers affected by dehydration or recent illness.
That is why clinicians often say things like “let’s repeat this in a few weeks” rather than instantly diagnosing a disease. They are not ignoring the result. They are checking whether the pattern persists.
The blood tests people most often see
Some blood tests are very specific. Many are more general. The ones most patients come across again and again are these:
full blood count, iron studies, vitamin B12 and folate, vitamin D, kidney function, liver function, glucose or HbA1c, cholesterol profile, thyroid function and inflammatory markers such as CRP or ESR.
Once you understand those groups, most everyday blood test reports start to look far less mysterious.
Full blood count: the one that gets ordered all the time
A full blood count (FBC) is one of the commonest blood tests in UK primary care and hospital medicine. It looks at the cells in your blood, especially red blood cells, white blood cells and platelets. The NHS and Lab Tests Online UK both describe it as a standard way of checking for problems such as anaemia, infection and some blood disorders.
If you see an FBC on your report, the main parts people notice are:
Haemoglobin (Hb) – this measures the oxygen-carrying protein in red blood cells. If it is low, that may suggest anaemia. Anaemia is not a diagnosis in itself; it is a clue. The cause might be iron deficiency, heavy periods, B12 or folate deficiency, chronic disease, blood loss, kidney disease or other problems.
Red blood cell indices such as MCV and MCH – these help doctors work out what type of anaemia may be present. A low MCV can point towards iron deficiency or thalassaemia trait, while a high MCV can happen with B12 or folate deficiency, alcohol use, liver disease, some medicines and other causes.
White blood cells (WBC) – these are part of the immune system. If raised, they may suggest infection, inflammation, recent stress on the body, smoking, steroid use or other causes. If low, they may need follow-up depending on the level, the type of white cells affected and whether the change is new.
Platelets – these help blood clot. Raised platelets can happen with inflammation, infection or iron deficiency, among other things. Low platelets may need further assessment depending on how low they are and whether there are symptoms such as bruising or bleeding.
A useful real-life example is the patient who is constantly tired and has heavy periods. Their FBC shows low haemoglobin and a low MCV. That pattern often pushes the clinician to look closely at iron deficiency. Another example is the person who had a bad viral illness last week and now has a mildly raised white count; that may be far less alarming than it looks on paper.
If the issue turns out to be iron-related, it may also connect naturally with some of your existing content such as heavy periods: causes, tests and treatment, fibroids: symptoms, heavy bleeding and treatment and endometriosis: symptoms, diagnosis and treatment.
Ferritin and iron studies: why “low iron” is not one simple thing
When patients say “my iron was low”, they are often referring to ferritin, which is one of the most useful markers of iron stores. Ferritin is especially helpful because it can fall before full anaemia develops. In other words, you can have low iron stores and feel tired, washed out, breathless or headachy before haemoglobin drops far enough to show classic anaemia.
Ferritin, however, is not perfect. NHS laboratory sources note that it can rise during inflammation or illness because it behaves as an acute phase reactant. That means a ferritin result that looks “normal” may sometimes be misleading if someone is inflamed or unwell at the time.
Other iron-related tests may include serum iron, transferrin saturation and total iron-binding capacity, but in day-to-day UK practice ferritin and the FBC often do much of the heavy lifting.
A classic example is a woman with very heavy periods, restless legs, hair shedding and fatigue. Her haemoglobin may still sit just inside range, but ferritin is low. That does not mean the symptoms are imaginary or that “everything is fine”. It often means the iron stores are running down before more obvious anaemia has developed.
For readers dealing with symptoms that may connect to iron deficiency, your women’s health guides on women’s health symptoms and treatment, menopause symptoms and HRT treatment and vaginal discharge: what’s normal and what’s not can help them think about the wider symptom picture.
Vitamin B12, folate and vitamin D: common tests, often misunderstood
These tests are frequently ordered for tiredness, dietary concerns, nerve symptoms, low mood, anaemia investigation or general “I’m not feeling right” symptoms.
Vitamin B12 and folate are especially relevant if someone has macrocytic anaemia, tingling, numbness, mouth ulcers, dietary restriction, malabsorption or certain gut conditions. Low B12 is one of those results that should be interpreted carefully, because symptoms and severity do not always match the number neatly.
Vitamin D is a little different. It is commonly tested, often discussed, and widely supplemented, but it can easily become a source of confusion. Low vitamin D can contribute to bone pain, muscle aches and tiredness, but many symptoms people blame on vitamin D are not specific to it. It is important not to force every vague symptom into one explanation just because a vitamin level is borderline.
These tests matter, but they are best interpreted alongside symptoms, diet, gut health, medications and the FBC rather than as standalone magic answers.
Kidney function: creatinine, urea and eGFR
Kidney blood tests cause a lot of unnecessary alarm because patients often focus on eGFR without understanding what it actually means.
The main kidney-related markers you will often see are:
Creatinine – a waste product filtered by the kidneys.
eGFR – an estimated measure of kidney filtering function, calculated from creatinine and other factors.
Urea – another waste product that can be affected by hydration and other factors.
The NHS guidance on chronic kidney disease diagnosis explains that eGFR is used to estimate kidney function and classify chronic kidney disease stages, but the important patient point is this: one slightly reduced eGFR does not automatically mean you have serious kidney disease. Doctors usually interpret it alongside creatinine, urine tests such as ACR, blood pressure, diabetes status, age and whether the result is stable over time.
A good example is the muscular patient whose creatinine is a bit high because they have more muscle mass, or the mildly dehydrated person whose kidney numbers look worse on a hot day or during illness. Context matters enormously here.
Patients who also want to understand the bigger cardiovascular picture may find it helpful to read your related articles on high blood pressure, home blood pressure monitoring and cardiovascular risk.
Liver function tests: helpful, but not as simple as they sound
“Liver function tests” or LFTs are another group that frightens people because they sound like a direct verdict on how well the liver is working. In reality, some of these tests are really markers of liver irritation or patterns of bile flow rather than a single yes-or-no test of liver health.
Common LFT components include:
ALT and AST – enzymes that may rise when liver cells are irritated or injured.
ALP – which can rise with bile duct issues but also with bone-related processes.
Bilirubin – a yellow pigment that can rise in liver disease, bile duct problems and some benign conditions such as Gilbert’s syndrome.
Albumin – a protein made by the liver, which can be low for several reasons including inflammation, kidney loss, malnutrition and liver disease.
The NHS notes that blood tests used to assess the liver are called liver function tests, but that they can be normal in some stages of liver disease and abnormal for more than one reason. That is a very useful reminder: abnormal LFTs do not always mean major liver damage, and normal LFTs do not prove that every liver-related problem is impossible.
A common real-world scenario is the patient whose ALT is mildly raised after recent illness, weight gain, alcohol intake or medication use. Another is the patient with isolated bilirubin elevation who turns out to have benign Gilbert’s syndrome rather than a dangerous liver problem. The pattern matters more than one scary-looking flag.
If digestion symptoms are also part of the story, you have relevant internal articles on digestive health symptoms and common conditions, stomach ulcers, gallstones and IBD explained.
HbA1c and glucose: understanding diabetes and prediabetes results
These are among the most important numbers people see because they often affect long-term health decisions.
Glucose tells you what your blood sugar is at that moment, usually fasting or non-fasting depending on the test.
HbA1c reflects average blood glucose over roughly the previous two to three months. That is why it is such a useful test for diagnosing and monitoring diabetes. NICE patient information explains that HbA1c is a measure of average blood glucose over that time period, not just a snapshot on one day.
In practice, patients often hear terms like “normal”, “prediabetes” or “diabetes range”. The important point is not just the label but what happens next. A result in the prediabetes range does not mean inevitable diabetes. It is often a moment to look closely at weight, diet, sleep, activity and longer-term risk. A result in the diabetes range may need confirmation and proper follow-up depending on symptoms and the clinical situation.
A very common example is the person who feels completely well, has a routine test, and is told their HbA1c is higher than expected. That can be unsettling, but it is also exactly the sort of result that can be useful early, before symptoms become obvious.
Cholesterol and lipids: more than one number, and not a moral verdict
Cholesterol results are often oversimplified. Patients want one answer: good or bad. But a lipid profile is more nuanced than that. It may include total cholesterol, LDL cholesterol, HDL cholesterol and triglycerides.
The NHS blood tests overview says a lipid profile is used to check cholesterol levels and assess risk of conditions such as cardiovascular disease and stroke. But the number that matters most is not always just total cholesterol. Doctors usually interpret the result alongside age, blood pressure, diabetes, smoking, family history and overall cardiovascular risk.
This is why one person with “slightly high cholesterol” may simply be advised about diet and exercise, while another may have a more serious conversation about statins and broader risk reduction.
You already have strong related content here, and this new article should naturally link to cholesterol test results explained, high cholesterol, statins explained and how to reduce your risk of heart attack and stroke.
Thyroid blood tests: TSH, T4 and why symptoms matter so much
Thyroid testing is another area where people often obsess over the number without understanding the relationship between the markers.
The most common tests are:
TSH – thyroid-stimulating hormone, produced by the pituitary gland.
Free T4 – thyroxine, one of the main thyroid hormones.
Sometimes T3 is also measured, but not always.
The NHS thyroid testing information explains that thyroid function blood tests check hormones such as TSH, T3 and T4, and that patterns in these help diagnose overactive or underactive thyroid conditions. In broad terms, a raised TSH with a low free T4 often points towards primary hypothyroidism, while a low TSH with raised thyroid hormones points in the opposite direction.
But mild thyroid abnormalities can be less straightforward. A slightly raised TSH does not always mean immediate treatment. Sometimes it means monitoring. Sometimes it depends on symptoms, pregnancy plans, antibody tests, age and whether the result is persistent.
This is one reason thyroid blood tests should never be read as isolated internet trivia. They work best when tied to the symptom picture: fatigue, weight change, constipation, palpitations, tremor, menstrual changes, hair changes, feeling unusually cold or hot.
That symptom overlap is also why readers may move from this article into your broader hormone-related content such as menopause symptoms and HRT treatment, testosterone deficiency in men and PCOS symptoms, diagnosis and treatment.
CRP and ESR: useful clues, but non-specific ones
CRP and ESR are inflammation markers. Patients often see them because a GP is checking for infection, inflammatory disease, or whether there may be more going on behind symptoms such as pain, fever, bowel problems or unexplained fatigue.
These tests can be useful, but they are not diagnosis machines. A raised CRP may happen with infection, inflammatory conditions, tissue injury and several other causes. A normal CRP does not rule out every important condition. An ESR can stay raised for broader reasons and is often slower-moving.
This is one of the best examples of why blood tests are pattern-recognition tools. A CRP is most useful when combined with symptoms, examination and the rest of the blood panel.
Coeliac tests, gut tests and disease-specific bloods
Some blood tests are more focused. Coeliac screening, autoimmune antibodies, hormone panels, PSA, reproductive hormone testing, hepatitis screens and other specialist bloods are often ordered for specific clinical questions. These are harder to interpret outside context because their value depends heavily on why they were ordered in the first place.
For example, a coeliac screen is not the same as “a digestion blood test”, and a PSA is not a simple yes-or-no cancer test. A fertility-related hormone panel may mean something different depending on age, sex, menstrual cycle timing or medication use. This is why specialist bloods are often the least suitable for DIY interpretation online.
You already have good internal pages that can support this kind of follow-up reading, including coeliac disease, men’s health symptoms and treatment, women’s health symptoms and treatment and male infertility and low sperm count.
Why results can be abnormal even when nothing serious is wrong
This is a point that deserves repeating because it saves so much unnecessary fear.
Blood results can shift because of temporary illness, dehydration, alcohol, exercise, supplements, menstrual bleeding, pregnancy, recent infection, lab variation, medication, fasting status, stress on the body and timing. Some numbers move for reasons that are important but not dangerous. Some look dramatic but are expected in context. Some need repeating before anyone can say what they really mean.
A person who had a stomach bug may have temporarily concentrated blood results. A person who exercises hard before a test may nudge some enzymes upward. A person taking iron tablets may change the look of iron-related results. A woman with a very heavy period may temporarily shift several markers at once. None of that means doctors dismiss the test. It means interpretation requires real life.
What doctors usually look for, beyond one number
Patients often imagine doctors read blood tests line by line, reacting to each red arrow. In reality, they usually look for patterns.
Low haemoglobin plus low MCV plus low ferritin suggests one sort of problem. A high TSH plus low free T4 suggests another. Raised cholesterol plus high blood pressure plus diabetes risk points to a much bigger cardiovascular picture than cholesterol alone. Mildly abnormal liver enzymes plus raised BMI plus metabolic risk factors may point towards fatty liver rather than a sudden crisis.
That pattern-based thinking is the bridge between numbers and actual medicine.
When a blood test result should make you chase follow-up
Not every abnormal result is urgent, but some definitely deserve proper follow-up. You should be more proactive if:
the abnormality is significant rather than borderline; several related results are abnormal together; the result fits an ongoing symptom pattern; the abnormality is new and unexplained; you have persistent symptoms despite being told results are “mostly fine”; or the surgery has advised repeat testing, review or medication changes and you are not sure what happens next.
This is especially true for marked anaemia, clearly abnormal kidney function, substantially raised liver tests, diabetes-range glucose results, significant thyroid abnormalities, very low B12, unexplained high inflammatory markers, or any pattern linked with worrying symptoms such as weight loss, bleeding, jaundice, black stools, chest symptoms or severe fatigue.
If getting reviewed is the problem, your readers may benefit from how to get a GP appointment quickly in the UK, private GP services in the UK and when to see a pharmacist instead of a GP.
Questions worth asking after you get blood test results
If you want to get more out of the appointment or message exchange, these are better questions than “Is this bad?”
What was the test looking for in the first place? Which result matters most? Is the abnormality minor or more meaningful? Could it be temporary? Does it need repeating? Does it fit my symptoms? Are there likely causes you are considering? Do I need treatment, monitoring, another test, or no action at all? What symptoms should prompt me to come back sooner?
Those questions usually lead to a far more useful answer than simply staring at the numbers yourself.
Why private tests can be helpful but also confusing
Private blood tests can be useful for access and convenience, but they can also create unnecessary worry if you order large panels without a clear reason. The more tests you do, the more likely it is that one or two numbers will fall just outside range by chance alone. That can generate anxiety, repeat testing and over-interpretation.
This does not mean private testing is a bad idea. It means results still need clinical interpretation. A huge spreadsheet of biomarkers is not automatically better than a smaller, more targeted panel ordered for a sensible reason.
Your broader guides on NHS vs private healthcare in the UK and how hospital referrals work in the UK can help readers understand where blood tests fit into the bigger healthcare journey.
The bottom line
The best way to understand blood test results is not to treat them like exam marks. They are not grades and they are not verdicts on whether you are healthy or unhealthy. They are pieces of clinical information. Some are reassuring, some are clues, some need repeating, and some point clearly towards a diagnosis when placed in the right context.
If you remember only a few things, make them these: a result slightly outside range is not always a problem; a “normal” result does not rule out every condition; patterns matter more than single numbers; and the reason the test was ordered matters just as much as the result itself.
Once you start looking at blood tests that way, they become much less intimidating — and much more useful.
Frequently asked questions
What does it mean if a blood test result is marked high or low?
It means your result sits outside that laboratory’s reference range. It does not automatically mean something serious is wrong. The importance depends on how far outside range it is, whether other related results are also abnormal, and whether it fits your symptoms and medical history.
Can blood tests be abnormal for harmless reasons?
Yes. Mild abnormalities can happen because of dehydration, recent illness, inflammation, medication, exercise, alcohol, menstruation, pregnancy, supplements and normal biological variation. That is one reason repeat tests are often useful.
What is the most common blood test?
One of the most common is the full blood count, or FBC. It checks red blood cells, white blood cells and platelets, and is often used to look for anaemia, infection or broader blood-related problems.
What is ferritin and why do people talk about it so much?
Ferritin reflects iron stores and is especially useful when doctors are checking for iron deficiency. It can fall before full anaemia develops, which is why people can have symptoms of low iron even when haemoglobin is not dramatically low.
Is a low eGFR always a sign of kidney disease?
No. eGFR needs context. A mildly reduced result may need repeat testing and interpretation alongside creatinine, urine tests, age, blood pressure and the wider clinical picture. One isolated number does not always equal chronic kidney disease.
What is HbA1c?
HbA1c is a blood test that reflects your average blood sugar over the previous two to three months. It is commonly used to diagnose and monitor diabetes and prediabetes.
Why would my doctor repeat a test instead of treating it straight away?
Because some abnormalities are temporary or need confirmation. Repeating a test helps show whether a result was a one-off blip or part of a real pattern that needs action.
Should I worry if my results are normal but I still have symptoms?
Not necessarily worry, but do not assume the story ends there. Blood tests are helpful, but they do not detect every condition. If symptoms persist, worsen or clearly affect daily life, it is reasonable to go back and ask what the next step should be.
When should I urgently follow up blood test results?
You should seek prompt medical advice if a clinician has told you a result needs urgent review, or if abnormal results come with concerning symptoms such as chest pain, severe shortness of breath, jaundice, black stools, heavy bleeding, severe weakness, marked weight loss or confusion.