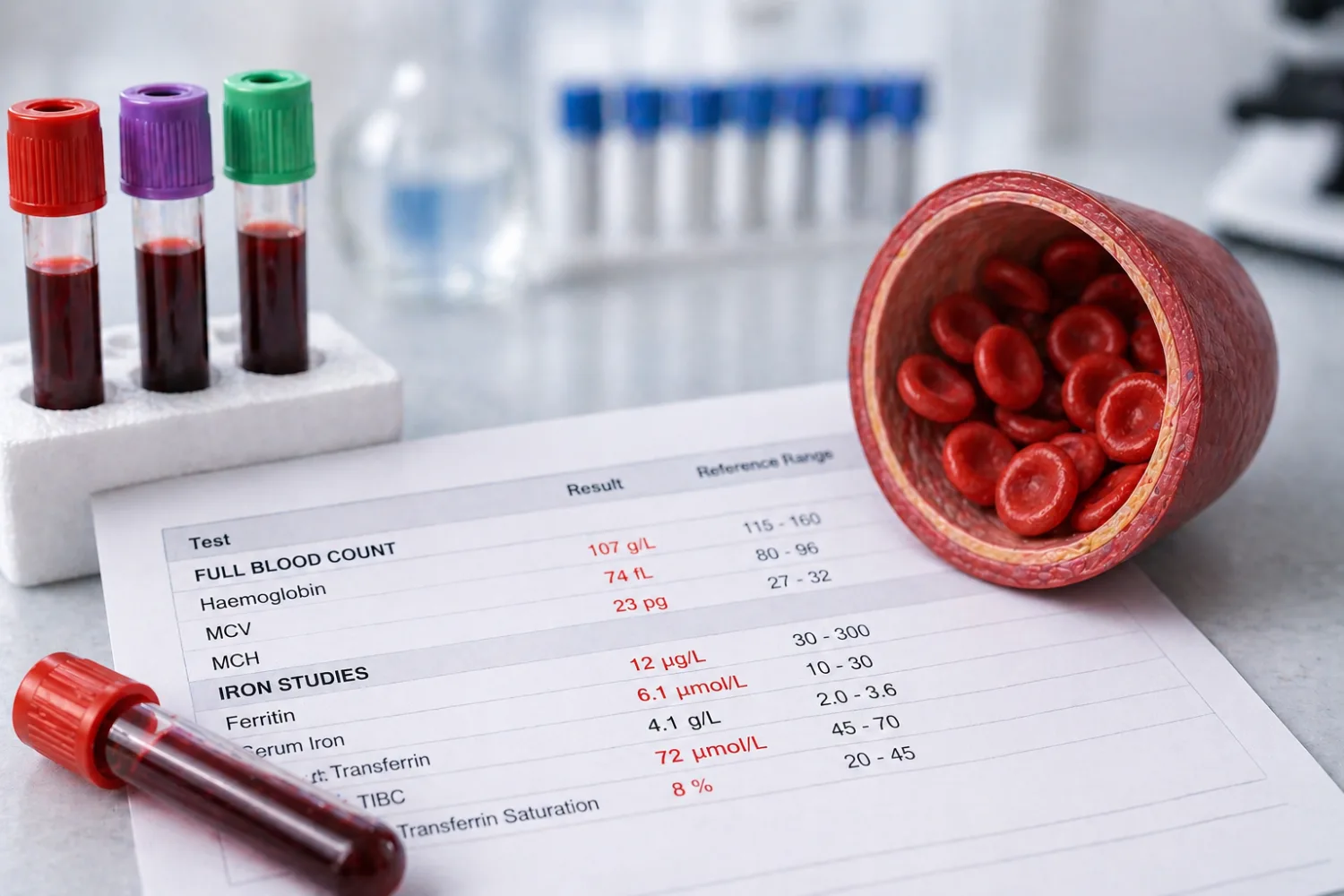
Iron blood tests are some of the most confusing results patients see. Someone is told their haemoglobin is low, or their ferritin is low, or that their iron is “fine” but they might still be iron deficient. Another person sees a normal full blood count and assumes iron is not the problem, only to find later that their ferritin was low all along.
The confusion usually comes from one simple fact: iron deficiency, low iron stores and anaemia are related, but they are not exactly the same thing. A person can have low iron stores before full anaemia develops. A person can have anaemia that is not caused by iron deficiency. And a ferritin result can be affected by inflammation, which sometimes makes interpretation trickier than patients expect. NICE CKS notes that a serum ferritin below 30 micrograms/L confirms iron deficiency, but also explains that ferritin can be more difficult to interpret when inflammation is present.
This guide explains the blood test results UK patients most often see when iron deficiency or anaemia is being investigated, including haemoglobin, ferritin, serum iron, transferrin, TIBC and transferrin saturation. It also explains why one low result does not always give the full answer, what common patterns doctors look for, and when follow-up matters.
What doctors are usually checking when they suspect iron deficiency
When a GP suspects iron deficiency or anaemia, the first test is often a full blood count, or FBC. The NHS says a blood test called a full blood count is usually done to see whether the number of red blood cells is normal, and it is a standard test when iron deficiency anaemia is suspected.
If the FBC suggests anaemia, or if symptoms strongly point towards iron deficiency, doctors may then look at ferritin and sometimes a broader iron profile. Lab Tests Online UK explains that an iron test panel may include serum iron, ferritin and transferrin to assess iron levels in the body and help diagnose conditions such as iron deficiency anaemia or iron overload.
This is why a simple comment like “your iron was low” is often too vague to be useful. The doctor may be talking about ferritin, haemoglobin, transferrin saturation or the overall picture rather than one single test called “iron”.
What anaemia actually means
Anaemia means there is not enough haemoglobin in the blood. Haemoglobin is the protein in red blood cells that carries oxygen around the body. When haemoglobin is low, people may feel tired, short of breath, light-headed, weak, cold or unable to exercise as well as usual.
But anaemia is not a diagnosis on its own. It is a finding. Iron deficiency is one common cause, but not the only one. Vitamin B12 deficiency, folate deficiency, chronic inflammation, kidney disease, blood loss and other conditions can also cause anaemia. The NHS explains that iron deficiency anaemia is only one type of anaemia, and NHS guidance on vitamin B12 or folate deficiency makes clear that these deficiencies can also cause anaemia based on blood test results.
This is the first key point: low haemoglobin does not automatically mean low iron, and low iron does not always mean haemoglobin has dropped yet.
Haemoglobin: the number people notice first
Haemoglobin, often shortened to Hb, is one of the most important parts of the full blood count. If it is low, that tells the clinician you are anaemic. The NHS says the FBC checks whether the number of red blood cells is normal and is used in the diagnosis of iron deficiency anaemia.
A common real-life example is someone who has been tired for months and finally has blood tests. Their haemoglobin is low, which confirms anaemia. That does not yet explain why, but it tells the doctor the problem is real and needs explaining.
Another common example is someone with heavy periods whose haemoglobin is still within the lab range, but only just. If ferritin is low as well, they may be iron deficient even before obvious anaemia becomes established. That is why doctors often look beyond the haemoglobin alone.
This guide links naturally with your broader article on how to understand blood test results, and also with symptom-led pages such as heavy periods, fibroids and endometriosis.
Ferritin: often the most useful iron test
Ferritin is one of the most useful tests when doctors are checking iron stores. Lab Tests Online UK says a ferritin test measures the level of ferritin in the blood to assess how much iron the body has stored.
In practice, ferritin is often the test patients should pay the closest attention to when iron deficiency is suspected. A low ferritin usually means iron stores are low, even if haemoglobin has not yet dropped far enough to cause obvious anaemia. NICE CKS states that in all people, a serum ferritin level of less than 30 micrograms/L confirms iron deficiency.
This is why some people feel exhausted, foggy, breathless or notice hair shedding even though their full blood count is only mildly abnormal or still technically normal. Their iron stores may already be depleted.
But ferritin is not perfect. Ferritin can rise when inflammation or illness is present, because it behaves as an acute phase reactant. NICE CKS and RUH NHS guidance both note that ferritin is harder to interpret in the presence of inflammation.
That means a ferritin that looks “normal” on paper does not always completely rule out iron deficiency if someone is also inflamed or unwell.
Serum iron: useful, but often overinterpreted
Serum iron measures the amount of iron circulating in the blood at that moment. Lab Tests Online UK includes serum iron as part of a broader iron test panel used to assess iron levels in the body.
Patients often assume serum iron is the main iron result, but it can actually be one of the harder ones to interpret on its own. It can vary through the day and can be influenced by recent intake and other factors. That is why doctors usually interpret it as part of a pattern rather than in isolation.
A low serum iron can fit iron deficiency, but by itself it is often less useful than ferritin and transferrin saturation. Likewise, a serum iron that looks “normal” does not necessarily mean iron stores are fine.
TIBC and transferrin: how the body carries iron
TIBC stands for total iron-binding capacity, and transferrin is the protein that binds and transports iron around the blood. The NHS explains that a TIBC test measures the blood’s ability to attach itself to iron and transport it around the body, and that a transferrin test is similar. If you have iron deficiency anaemia, the NHS says your iron level will usually be low while your TIBC will be high.
Lab Tests Online UK similarly explains that TIBC, UIBC and transferrin tests assess the blood’s capacity to bind and transport iron and are used to help diagnose iron deficiency anaemia or iron overload disorders.
This sounds technical, but the practical meaning is fairly simple. When the body is short of iron, it often makes more room to bind and grab hold of any iron available. So TIBC tends to rise in iron deficiency.
Transferrin saturation: one of the most helpful pattern tests
Transferrin saturation, sometimes written as TSAT or TSATS, looks at how much of the iron-carrying protein is actually loaded with iron. It helps show how available iron is for the body to use.
Several UK guidance sources use transferrin saturation as part of iron deficiency assessment. For example, Coventry and Rugby GP Gateway notes that ferritin under 15 µg/L and/or transferrin saturation under 20% support iron deficiency, and other NHS pathways use similar cut-offs.
This can be especially useful when ferritin is not straightforward, such as when inflammation may be pushing ferritin up. A pattern of low transferrin saturation plus suggestive symptoms may strengthen the case for iron deficiency even when the ferritin is not dramatically low.
Iron deficiency without anaemia: why people can feel unwell before haemoglobin drops
This is one of the most important ideas for patients. Iron deficiency does not begin on the day haemoglobin becomes low. Iron stores can run down first, which is why ferritin may fall before full iron deficiency anaemia develops.
The NHS pregnancy iron guideline explains that in iron-deficiency anaemia, the most severe form of iron deficiency, there is shortage of iron stores, transport and functional iron, resulting in reduced haemoglobin in addition to low ferritin and low transferrin saturation.
In plain English, this means there is a spectrum:
first, low iron stores; then low available iron; then, if it continues, iron deficiency anaemia.
A good example is the patient with heavy periods, hair loss, restless legs and tiredness whose ferritin is low but haemoglobin is still within range. They may still be iron deficient even though they are not yet frankly anaemic.
What doctors look for on the full blood count
When anaemia is present, doctors also look at the size and appearance of red blood cells on the FBC. Iron deficiency often causes a microcytic pattern, meaning the red cells are smaller than usual. That may show up as a low MCV and sometimes a low MCH.
But again, patterns matter more than one isolated result. A low MCV with low ferritin points in one direction. A normal MCV with low ferritin may still be iron deficiency in an earlier stage. A high MCV points doctors more towards B12 or folate deficiency, alcohol effects, liver disease or other causes rather than simple iron deficiency. NHS guidance on vitamin B12 or folate deficiency anaemia confirms that these deficiencies are diagnosed from symptoms and blood test results and are a different cause of anaemia altogether.
Common causes of iron deficiency in adults
Once iron deficiency is identified, the next question is why. British Society of Gastroenterology guidance emphasises that iron deficiency anaemia is common and that the cause should be investigated rather than simply assuming it is dietary.
Common causes include heavy menstrual bleeding, pregnancy, reduced dietary intake, poor absorption, coeliac disease, inflammatory bowel disease and blood loss from the digestive tract. That is why low ferritin or iron deficiency anaemia often leads to questions about periods, bowel symptoms, acid-suppressing medication, diet and sometimes referral for further investigation.
This is why the result is often only the beginning of the conversation. You already have strong internal content that can support this journey, including coeliac disease, IBD explained, blood in stool and women’s health symptoms and treatment.
Why ferritin can be misleading when inflammation is present
Ferritin is a very useful test, but it is not infallible. NICE CKS specifically notes that ferritin is difficult to interpret when inflammation is present. RUH NHS guidance also highlights that ferritin rises as an acute phase reactant, which can mask iron deficiency.
This is one reason iron deficiency can be missed in people with chronic illness, inflammatory conditions or recent infection. A ferritin that looks “acceptable” might not tell the whole story if CRP or ESR is raised at the same time.
That is where a broader pattern, including transferrin saturation, full blood count and symptoms, becomes more useful than a single lab value.
What happens after iron deficiency is found
If iron deficiency anaemia is diagnosed, the NHS says treatment usually involves taking iron tablets prescribed by a GP and addressing the cause where possible.
Several NHS and UK guidance sources also emphasise follow-up blood tests. Manchester NHS guidance says the FBC and reticulocyte count can be checked after around 10 days to assess response, then again after several weeks to confirm recovery, while Barts Health guidance notes that FBC and ferritin should be rechecked after intravenous iron and then monitored if the deficiency recurs.
The important point for patients is that treatment is not only about getting the haemoglobin up. It is also about replenishing iron stores and understanding why the deficiency happened in the first place.
When iron results need more careful follow-up
Iron deficiency matters more when anaemia is significant, symptoms are marked, treatment is not working, or there is concern about an underlying cause such as gastrointestinal blood loss. British Society of Gastroenterology guidance gives particular weight to identifying causes of iron deficiency anaemia rather than treating numbers alone.
A poor response to iron replacement may mean the tablets are not being taken, not being absorbed well, or that the diagnosis is incomplete. Manchester NHS guidance specifically says that if haemoglobin initially responds and then stops improving, ferritin should be checked to see if secondary iron deficiency has occurred.
That is why persistent symptoms, recurrent low ferritin, or iron deficiency without an obvious explanation should not simply be left to drift.
Questions worth asking after iron blood tests
If you have been told your iron is low, ask which result is actually low. Was it haemoglobin, ferritin, serum iron or transferrin saturation? Do you have iron deficiency, iron deficiency anaemia, or just low iron stores so far? Does the result need repeating? Is there an obvious cause such as periods or diet, or do you need more investigation? If treatment is started, when should the blood tests be repeated?
Those questions are much more useful than simply asking whether your iron is “bad”.
The bottom line
Iron blood tests make more sense once you separate three ideas. Ferritin reflects iron stores. Haemoglobin shows whether you are anaemic. Serum iron, transferrin, TIBC and transferrin saturation help explain how iron is being carried and how available it is for use. NICE CKS, NHS guidance and Lab Tests Online UK all support this broader, pattern-based approach rather than relying on one number alone.
So if your ferritin is low but haemoglobin is still normal, that can still matter. If your haemoglobin is low, that does not automatically mean iron is the cause. And if the results are confusing, the right next step is usually not self-diagnosis but understanding the pattern and the cause.
Frequently asked questions
What does ferritin measure?
Ferritin reflects the body’s iron stores. A ferritin test measures the level of ferritin in a blood sample to assess how much iron the body has stored.
Can you have low ferritin without anaemia?
Yes. Iron stores can fall before haemoglobin drops enough to cause full iron deficiency anaemia. This is why someone can have symptoms of iron deficiency even if the full blood count is not yet clearly anaemic.
What ferritin level means iron deficiency?
NICE CKS states that a serum ferritin level below 30 micrograms/L confirms iron deficiency, although interpretation can be harder if inflammation is present.
What does transferrin saturation mean?
Transferrin saturation shows how much of the iron-carrying protein is loaded with iron. Low transferrin saturation supports iron deficiency, especially when considered alongside ferritin and the full blood count.
Why can ferritin be normal if I am still iron deficient?
Ferritin can rise in inflammation or illness because it is an acute phase reactant, which can sometimes make iron deficiency harder to spot.
What is the difference between low iron and anaemia?
Low iron usually refers to depleted iron stores or low available iron, often reflected by low ferritin or low transferrin saturation. Anaemia means haemoglobin is low. Iron deficiency can lead to anaemia, but the two are not identical.
What causes iron deficiency in adults?
Common causes include heavy menstrual bleeding, pregnancy, low dietary intake, poor absorption, coeliac disease, inflammatory bowel disease and blood loss from the digestive tract. UK gastroenterology guidance emphasises that the cause should be identified, not just treated empirically forever.
When should iron blood tests be repeated?
That depends on the severity, treatment and clinical situation, but NHS guidance commonly recommends repeat testing after treatment begins to check that haemoglobin and iron stores are improving.